This column contains a correction.
The concerns of some Senate Republicans about making the opioid epidemic worse have spilled out of their secretive negotiations for repeal of the Affordable Care Act (ACA), in the form of a fund to combat opioid addiction. A $45 billion fund in the Senate bill would reportedly be aimed at helping people with dependence on prescription opioids and illicit forms of the drug, but it would provide scant resources to address the epidemic. The fund also would not be able to undo the true costs of the repeal bill, would result in millions of Americans losing health insurance coverage, and could cause those still insured to lose access to substance use disorder treatment.
There were 2.66 million people in the United States with an opioid use disorder (OUD) as of 2015. The Centers for Disease Control and Prevention (CDC) reports that 33,091 people died from an opioid overdose in 2015. West Virginia had the highest opioid overdose death rate; about 36 out of every 100,000 people in the state died from an opioid overdose that year.
The epidemic shows no signs of stopping and, in fact, appears to be accelerating. A recent New York Times analysis based on preliminary data estimated that about 59,000 people died of a drug overdose last year, and that 2017 could be even worse. Given the continuing growth of OUD, we estimate that the total cost of coverage for people receiving treatment for OUD could reach $220 billion over the next decade.
More importantly, the Senate ACA repeal bill is not a substitute for the comprehensive health benefits currently available through Medicaid and the ACA marketplaces. The opioid fund included in that bill would not come close to mitigating harm from other parts of bill. Even if the entirety of the fund were available to cover low-income individuals being treated for OUD, $45 billion would provide only half of the $91 billion that would be available under the ACA for health coverage alone.
The high cost of opioid dependence
Opioid dependence is treatable but expensive condition. The cost of medication-assisted treatment (MAT) is about $5,500 per year. However, treatment of the addiction is only one element of the cost of caring for people with opioid dependence. Other health consequences come with much bigger price tags. Average charges for opioid overdose patients treated and released from the emergency department are $3,397 per visit, while those admitted to the hospital racked up an average $29,497 in charges per hospitalization. And hospital care for babies born suffering from opioid withdrawal—a problem becoming more common—costs an average of $66,700 per birth. Opioid use also drives the spread of other expensive health conditions. Recent outbreaks of HIV and the rise in Hepatitis C can be traced to needle-sharing among users of injectable opioids.
The cost of the opioid crisis reaches far beyond health care. It strains the justice system and families. The CDC researchers estimated that, in 2013 alone, the total economic cost of opioid overdose, abuse, and dependence was $78.5 billion, including costs of treatment, health care, criminal justice, and lost worker productivity.
A large part of Medicaid care for OUD is covered by federal dollars. National data from the 2015 National Survey on Drug Use and Health (NSDUH) show that adults with incomes below poverty are more likely to have an OUD than those with incomes above. A recent report by the nonpartisan Medicaid and CHIP Payment and Access Commission stressed that while Medicaid enrollees were also more likely to receive treatment than those with private insurance, many Medicaid enrollees with OUD still go untreated due to reasons including care shortages, lack of funding, and stigma. States that have adopted the ACA’s Medicaid expansion have been able to extend treatment to thousands more people.
Both the House and Senate repeal bills share common elements that would deepen the opioid crisis. By 2026, the House-passed bill would increase the number of uninsured by 23 million, including 14 million people who would have otherwise had Medicaid coverage under the ACA. It would essentially end the enhanced federal funding available for the ACA’s Medicaid expansion, which currently covers more than 11 million low-income adults, including 99,000 with an OUD. Even if the Senate chooses to delay the repeal of Medicaid expansion by a few years, by 2026 the effect would be practically the same. At the inaugural meeting of President Donald Trump’s commission on the opioid crisis last week, health care experts pleaded for preserving Medicaid expansion and against cuts to the program.
Just like the House bill, the Senate version would cap the federal spending on most Medicaid enrollees, forcing states to expend more of their own budgets or reduce benefits. And just like the House bill, the Senate version could also make it difficult for people with private coverage to obtain treatment for OUD by allowing state waivers of essential health benefits, including substance use disorder treatment. Prior to the ACA, only 45 percent of individual market plans covered substance use disorder treatment.
National coverage costs for people with OUD
The Senate version of the AHCA would reportedly set aside $45 billion for OUD treatment. But the bill’s resources would be far from the total cost of coverage for people with OUD, even including additional money for OUD treatment that might be available from the House-passed bill’s $15 billion maternity and mental health fund. The bill’s opioid treatment funding cannot substitute for comprehensive coverage.
Based on data on OUD prevalence and the costs of coverage, we calculated the total cost of comprehensive coverage for people with OUD over the next decade, as well as the funding the federal government would provide for coverage for low-income people with OUD under the ACA. Nationwide, 2.66 million people had OUD as of 2015. Of these, 1.37 million have incomes below 200 percent of the federal poverty level.
Currently, only about one in four people with OUD receives treatment, which implies that approximately 665,000 people with OUD, including 343,000 low-income individuals, were treated in 2015. Such treatment comes at a cost: On average, Medicaid beneficiaries with OUD cost about $11,000 per year on average, compared with $3,300 per year for the average Medicaid adult.
Both the number of people seeking treatment and the cost of care will certainly rise in the near future. Pharmacy claims data show that the number of buprenorphine prescriptions increased an average of 11 percent annually over the period 2012-2016, driven by increase in both OUD and in its treatment. Assuming that the number of people receiving OUD treatment continues to rise at that rate, the number of people treated for OUD would rise from 665,000 in 2015 to 2.1 million in 2026.*** We assume the cost of care would also rise, by an average of 5 percent annually, based on projections by the Congressional Budget Office. This means that by the year 2026, the annual cost of coverage for someone with an OUD would be nearly $20,000.
Based on these assumptions, we estimate that the total national cost of covering people treated for OUD from 2018 to 2026 would be $221 billion. The cost would be $41 billion in 2026 alone, nearly the same amount as the $45 billion Senate opioid fund. Moreover, our estimate does not include the cost of health care for people with OUD who do not undergo treatment. It also does not include nonhealth-care costs of the crisis, such as prevention efforts and public safety.
Although some of the costs of coverage for people with OUD would be borne by individuals and employers through private coverage, and under the ACA, we estimate that the federal government would pay a significant share. In the exchanges, the federal government covers about 80 percent of premium costs for individuals up to 400 percent of the poverty; the share of the premium covered would be even higher for individuals with incomes below 200 percent of the federal poverty level.* When people with OUD are eligible for Medicaid under the ACA’s expansion to low-income adults, the federal government covers about 90 percent of the costs of coverage, and states pick up the other 10 percent. For our estimate, we assumed that the federal government pays 80 percent of costs for low-income individual with an OUD.
We estimate that, under the ACA, the federal government would provide $91 billion over the next decade if all people under 200 percent of the federal poverty level receiving OUD treatment were covered by Medicaid or highly subsidized exchange plans. The Senate bill’s $45 billion fund would offer little more than half of this. Even if we were to assume that half, or $7.5 billion, of the House bill’s maternity and mental health fund would be devoted to OUD treatment, the American Health Care Act’s (AHCA) funding for opioid dependence would only amount to $52.5 billion.
Costs of coverage for opioid use disorder by state
A shortage of federal funding would burden states, and those where OUD is most common could be hurt the most. Drug overdose death rates and other metrics suggest that the prevalence of OUD and its treatment varies greatly by state. For example, 1.33 percent of the nation’s nonelderly adults had an OUD in 2015, while in Ohio the rate of opioid abuse and dependence is 3.6 percent among adults enrolled in Medicaid. Prevalence of OUD also varies with income and demographics. For example, tabulations for a variety demographic groups from the NSDUH show that among nonelderly adults nationally, about 0.7 percent of individuals ages 60 to 64 and about 0.8 percent of non-Hispanic black individuals had OUD in 2015. At the higher end, prevalence was nearly 1.7 percent among men and among individuals with incomes below 100 percent of the federal poverty level.**
We also calculated the approximate cost of care for individuals receiving treatment for OUD in 2026 by state. Prevalence data are available for few states, however, so we instead classified each state’s opioid use as high, medium, or low based on the number of opioid prescriptions relative to the population. While state-level data do exist for drug overdose deaths, such mortality rates reflect both OUD prevalence as well as the type of opioids involved in cases of overdose and abuse in a state. Historically, black tar heroin has been more common in western states, while deadlier powdered heroin is more popular east of the Mississippi.
We then assigned one prevalence rate for OUD to each category of state, while ensuring that the national prevalence would remain 1.33 percent in our estimates. We gave the 17 states in the middle third of the distribution the national prevalence rate of 1.33 percent. We modeled states in the lowest third as having 1 percent rate of OUD prevalence, close to the lowest OUD rates observed among demographic groups. For the highest one-third of states—which includes Kentucky, Ohio, and West Virginia—we set OUD prevalence at 2 percent; this is higher that observed in the tabulations of demographic groups nationally but substantially lower than the 3.6 percent prevalence of opioid abuse and dependence among Medicaid beneficiaries in Ohio.
We then multiplied each state’s population of nonelderly adults by the low, medium, and high prevalence rates to roughly estimate the number of people who had an OUD in 2015. Because national data show that only one in four people with OUD was treated in 2015, we assumed that one-quarter of people with OUD in each state received treatment in 2015. We projected our estimates of the number treated forward to 2026 using the same methodology as for our national estimate.
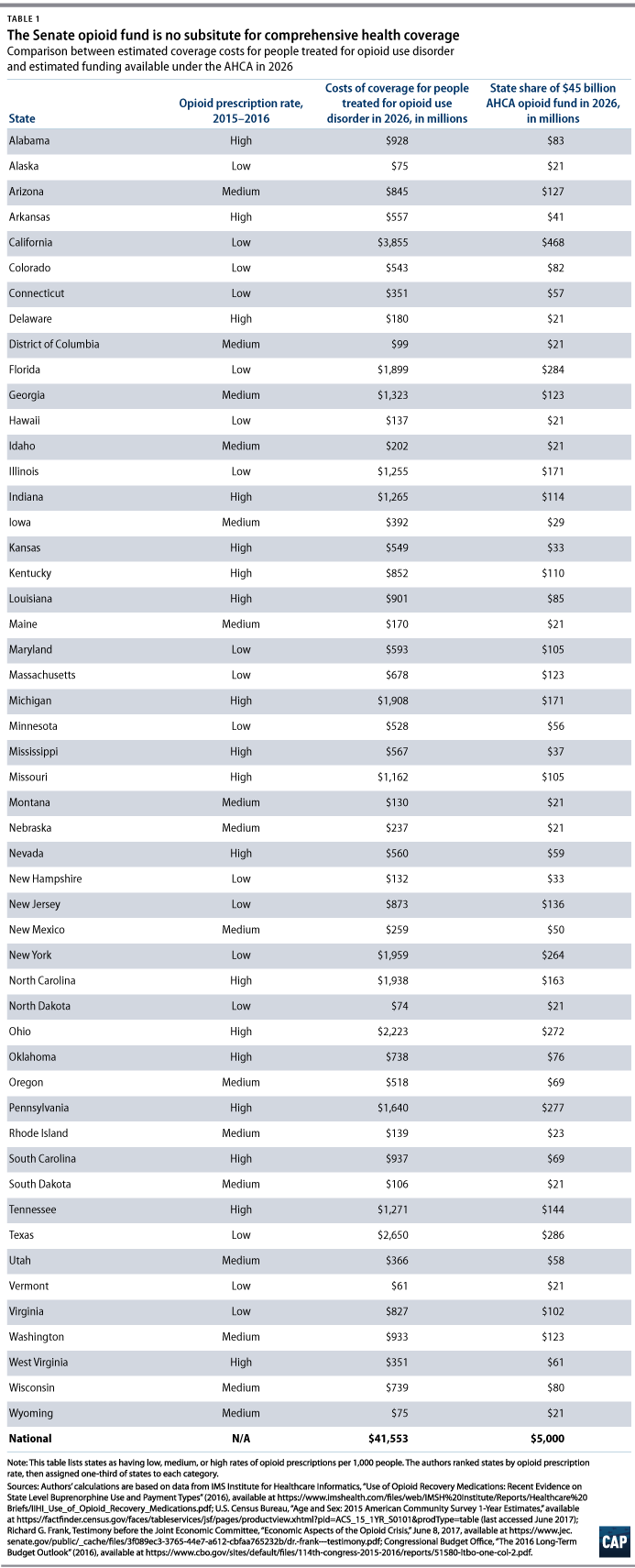
For comparison, we also estimated the federal funding that would be available from the Senate’s opioid fund. If the $45 billion fund were spread out evenly over the next nine years, $5 billion would be available annually from 2018 to 2026. Our table shows how much money would be available in each state if the fund allocation were the same as for the opioid crisis grants under the 21st Century Cures Act.
We estimate that by 2026 the cost of comprehensive coverage for all people treated for OUD in West Virginia and Ohio—two states currently mired in the epidemic—could reach $351 million and $2.2 billion, respectively. In our calculations, the Senate bill’s opioid fund could offer West Virginia $61 million and Ohio $272 million in 2026. Growth of treatment would generate staggering costs even in smaller states like Maine, where we estimate the total cost of coverage for people with OUD would be $170 million in 2026 compared with $21 million from the Senate fund.
Conclusion
The Senate bill’s $45 billion fund is merely a cover-up for the fact that the AHCA would strip millions of Americans of coverage while at the same time reducing the generosity of health insurance benefits. While more federal resources are needed to stem the opioid epidemic, the $45 billion fund offered up in Senate is not a stand-alone option. It is part of a package deal to reduce health insurance coverage and take away hundreds of billions of dollars of assistance to states, communities, and individuals in the face of a growing crisis.
Emily Gee is a health economist at the Center for American Progress. Richard G. Frank is the Margaret T. Morris professor of health economics in the Department of Health Care Policy at Harvard Medical School.
* Federal premium tax credits covered an average of 78 percent of the gross premium for all people who selected in 2017 in states using the HealthCare.gov enrollment platform and qualified for premium tax credits. People with incomes below 200 percent of the federal poverty line can also qualify for federal cost-sharing reduction subsidies, which raise the actuarial value of silver-tier plans to 87 and 94 percent.
** Tabulations of prevalence by Richard Frank and Carrie Fry using the 2015 National Survey on Drug Use and Health.
***Correction: June 26, 2017: This column has been corrected to accurately state the estimates of the total number of people treated for OUD. The number of total treated people for OUD is estimated to be 665,000 in 2015 and 2.1 million in 2026; the number of people treated for OUD who have incomes below 200 percent of the federal poverty level is 343,000 in 2015 and 1.1 million in 2026.