This week Axios reported that the emerging Senate bill to repeal the Affordable Care Act (ACA) will allow states to waive coverage of essential health benefits for small employer and individually purchased plans. In waiver states, this cut in benefits would be catastrophic for people who are sick or have a pre-existing condition and need prescription drugs, treatment for opioid addiction, or other services that could be excluded.
But the waivers would have a much broader impact, affecting millions of workers with employer coverage in every state—even nonwaiver states. As The Wall Street Journal reported, the waivers of essential health benefits would also eviscerate important financial protections that apply to large employer plans.
The Center for American Progress combined the results of a survey by Willis Towers Watson and census data to estimate the number of people with employer-based coverage who would be affected in each state. Nationally, we estimate that the Senate bill would erode or eliminate financial protections for about 27 million workers and their dependents.
The link between essential benefits and financial protections
The ACA bans plans from imposing annual and lifetime limits, which put caps on coverage for each year and over a lifetime. Prior to the ACA, 59 percent of workers were enrolled in an employer plan that had a lifetime limit. Such limits were commonly set as low as $1 million. For people with cancer or other diseases that require expensive drugs, or families with a newborn who starts life in the neonatal intensive care unit (NICU), these types of limits on coverage often resulted in bankruptcy.
The ACA’s ban on annual and lifetime limits applies with respect to essential health benefits, but does not apply with respect to other benefits. This means that if a benefit—such as coverage of maternity care or prescription drugs—were no longer considered an essential health benefit, the ACA’s ban would no longer apply with respect to that benefit. Plans could then impose a lifetime limit on coverage of prescription drugs, for example. If a waiver state chose to eliminate essential health benefits entirely, the ACA’s ban on annual and lifetime limits would also effectively be eliminated.
Importantly, under current regulations a large employer can choose to apply any state’s standard for essential health benefits for purposes of determining the scope of the ACA’s ban. Under the ACA, an employer’s choice of state standards is trivial because federal regulations require that all states’ essential health benefits include 10 core services. But under the Senate repeal bill, a large employer could choose the waiver state that provided it with the most flexibility on benefits. That choice would affect all the firm’s employees, regardless of whether they lived in waiver states, and they could face annual and lifetime limits on services that had previously been classified as essential.
The nonpartisan Congressional Budget Office recently confirmed that the bill’s waivers for essential health benefits would have this broader impact on employer plans:
For the large-group market, which generally consists of employers with more than 50 employees, current regulations allow employers to choose the EHB benchmark plan of any state in which they operate. Because of those regulations, a large employer operating in multiple states, including one that elected an EHB waiver, could base all of the plans it offers on the EHB requirements in a state with the waiver. That decision could allow annual and lifetime limits on benefits not included in the state’s EHBs.
Suppose that Utah obtains a waiver that eliminates all essential health benefits. Walmart, which is headquartered in Arkansas but has operations in all 50 states, could choose to apply Utah’s standard—or lack thereof—to all of its plans for all of its employees. In this indirect way, Walmart could impose annual and lifetime limits on any benefit for all of its employees nationwide.
Estimating the impact
Some may argue that large employers would not seek to reinstate such limits because they want to attract a talented workforce—and benefits are a major part of the compensation package. But the long-term trend indicates that employers are increasingly shifting health care costs to their employees, and limits were a tool that many employers used to contain costs prior to the ACA.
According to a recent survey of large employers by Willis Towers Watson, 20 percent said they would impose annual limits and 15 percent said they would impose lifetime limits if ACA protections were repealed. The Center for American Progress applied these percentages to estimates of people enrolled in employer-sponsored plans in each state.
We used American Community Survey data to estimate the total number of nonelderly people in each state whose primary coverage was employer-sponsored insurance in 2015. We then subtracted out enrollment in the small-group market according to administrative data for that year to obtain the number covered by large employers. We assumed that firms of a variety of sizes would impose limits if allowed, and that among those covered by employer-sponsored coverage, 20 percent of enrollees would face annual limits and 15 percent would face lifetime limits.
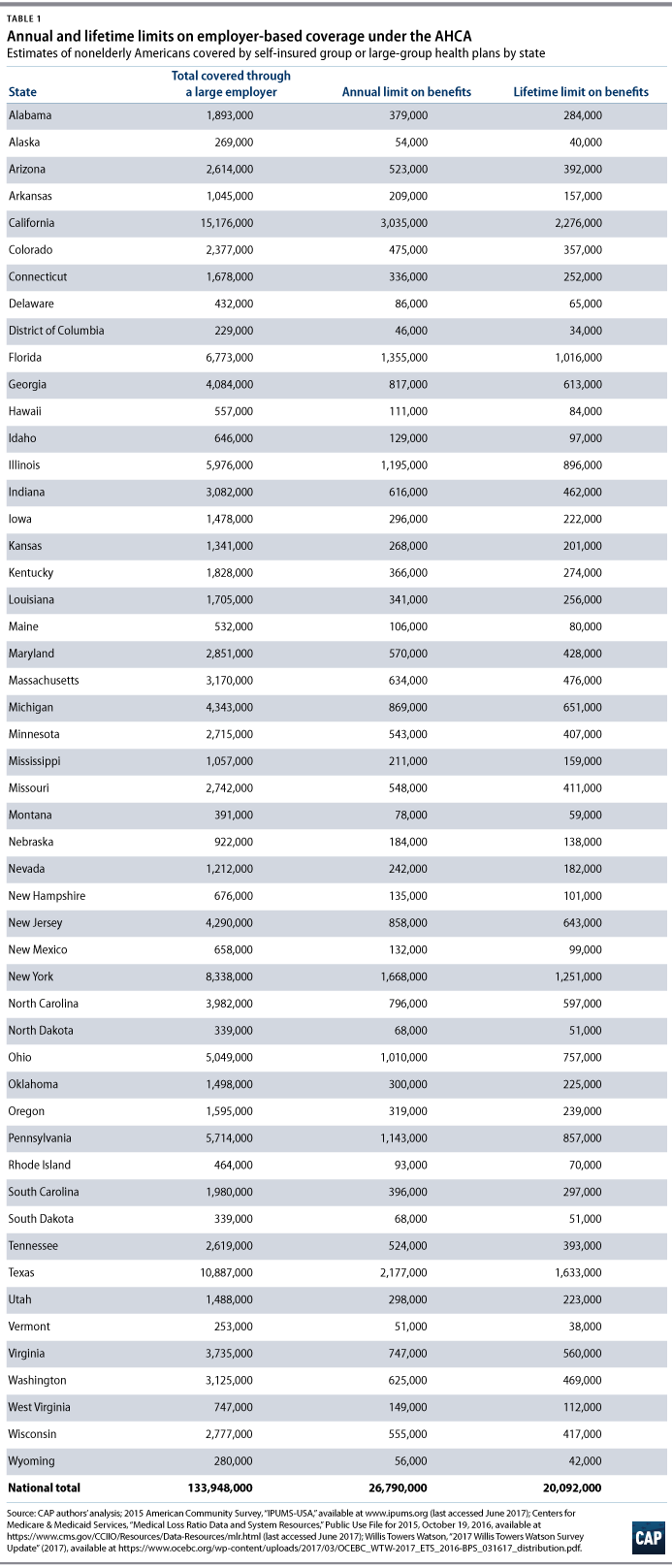
Nationwide, we estimate that the essential health benefit waivers would result in annual caps on benefits for nearly 27 million Americans with employer-based coverage. About 20 million people with employer-based coverage would face lifetime limits on coverage. Estimates by state are shown in Table 1.
Conclusion
The comedian Jimmy Kimmel recently shared the story of how his son was born with a life-threatening congenital heart defect, but, after being whisked away to surgery, survived. Tearfully, Kimmel said he hoped that any family in a similar situation would be able to receive the same level of care. Not long after, Sen. Bill Cassidy (R-LA) declared that any health bill should have to pass a “Jimmy Kimmel test.” The senator, in an appearance on Kimmel’s show, concurred with the Kimmel’s summary of the test: “No family should be denied medical care for an emergency or otherwise because they can’t afford it.”
As long as the Senate bill includes essential health benefit waivers, it will fail that test. The Republican bill’s waivers of essential health benefits threaten coverage not just for the individual market but also for the roughly 134 million Americans covered through large employers. Unlimited coverage for basic services like mental health, prescription drugs, and maternity coverage could disappear. Without it, cancer patients would not be able to access life-saving drugs, families would not be able to help a loved one obtain substance-abuse treatment, and new mothers would take home both babies and medical debt.
For too long, many American families—even those with health insurance—were just one illness away from bankruptcy, or faced the prospect of forgoing care for conditions excluded from coverage. The Senate must not return Americans to that time.
Topher Spiro is the vice president for health policy and a senior fellow for economic policy at American Progress. Emily R. Gee is the health economist for the Health Policy team at American Progress.