Erin Welch wrote this report in memory of her brother, Sean Francis Welch.
Introductory letter
For nearly a decade, our nation has watched the tragedy of the opioid crisis unfold. Americans are now all too familiar with the staggering statistics on opioid overdoses, which resulted in nearly 50,000 deaths in 2017 alone.1 Stories of grief and devastation abound from the communities hardest hit by this epidemic. Without a doubt, our city of Dayton, Ohio, has been hit harder than most by the opioid crisis. But most accounts of our adversity stop short of answering the most important question: What happened next?
To tell the full story, the city of Dayton teamed up with the Center for American Progress through the Mayors for Smart on Crime initiative to document our community’s response to turn the tide on the opioid crisis. This report highlights how a midwestern city at the center of the storm became a national model for stemming opioid-related overdoses. It shows how a community came together to face down an epidemic, mounting a creative and compassionate response that has saved countless lives. And it charts a roadmap for other city leaders to follow so they too can effectively meet the needs of residents affected by addiction.
When we began our work in Dayton, there was no blueprint for treating a substance misuse epidemic because the United States has never treated addiction as it treats other chronic illnesses. Our country’s long history of mishandling substance misuse culminated with the crack epidemic of the 1980s, when the war on drugs policy agenda took hold at all levels of government and led to the mass criminalization of communities of color. When the opioid epidemic surfaced in the early 2010s, it was clear that the country needed to take a smarter approach that treats substance misuse like a disease—not a crime.
It was in this context that Dayton waded in: innovating, trying, failing, and trying again. And while nobody will tell you that the problem is solved, our community has made enormous strides. The region was once considered the epicenter of opioid-related fatalities, with 378 overdose deaths in the first half of 2017 alone. But by June 2018, that number had been cut significantly with only 132 overdose-related deaths—a 65 percent reduction over the same period just the year before. As opioid misuse continues to spread to cities and towns nationwide, our model is one that other cities can—and should—learn from.
This report provides an analysis of the most effective strategies employed in Dayton and Montgomery County, outlining best practices for deploying local resources to treat a substance misuse crisis. Across the many interventions described in this report, several key themes and lessons emerge:
- Harm reduction services, such as syringe exchange programs, must be made available to people who are in active addiction and not ready to enter treatment. These services are integral to saving lives and reducing the spread of disease.
- Addiction must be treated as a disease, not a criminal act. This requires educating all stakeholders on the nature of the disease, including the likelihood of relapse, to ensure interventions reflect this understanding.
- Purposeful and rapid data collection, distribution, and analysis drives effective responses.
- Barriers must be broken down between community members, government agencies, county and city officials, the business sector, and local nonprofits to enable a coordinated effort. Interventions and endeavors often overlap, so everyone must be prepared to dive in collaboratively.
- Anyone working with people in active addiction must be nonjudgmental, immensely patient, and willing to combat the stigma of addiction within the community.
Though our work is far from done, Dayton’s story is a hopeful one. We have built a long-term path forward, setting up an infrastructure that positions our city to respond to residents’ substance misuse needs—from the opioid epidemic and beyond. No matter what substance use issues may arise in the future, Dayton will be prepared to respond with compassion, resilience, and determination.
Nan Whaley, Mayor, City of Dayton
Ed Chung, Vice President of Criminal Justice Reform, Center for American Progress
Executive summary
In 2017, a staggering 72,000 Americans died of drug overdoses—nearly 200 people every day.2 More than two-thirds of those fatalities, nearly 50,000 deaths, were caused by opioids. The number of opioid-related deaths has more than doubled in the past five years alone, rising to the level of a national epidemic.3
Dayton, Ohio, is one of the communities that the opioid crisis has hit hardest. Home to 140,000 residents, Dayton is the largest city in southwestern Ohio’s Montgomery County. Since 2011, Montgomery County has had the highest rate of overdose deaths in Ohio—a state whose opioid fatality rate consistently ranks among the highest in the nation.
But even as opioid misuse continues to spread nationally, the Dayton region has seen a precipitous drop in overdose-related fatalities. By midyear 2018, overdose deaths were down by 65 percent from the year before. Montgomery County recorded 132 overdose deaths in the first six months of 2018, compared with 378 overdose deaths during the same period in 2017.
The key to the city’s success was its willingness to take a compassionate new approach that was rooted in a collective impact model and driven by data. Facing unprecedented loss of life, the community rejected outdated strategies that criminalize addiction in favor of treating addiction like the disease that it is. Dayton and the surrounding region came together to embrace an all-hands-on-deck mentality, breaking down barriers between city and county government agencies, nonprofit organizations, businesses, and more. Dayton was one of the first jurisdictions in the state to declare a state of emergency in response to the opioid epidemic—a move that allowed the city to launch harm reduction initiatives such as syringe exchanges, which prevent the spread of disease and limit public disposal of used syringes. Dayton was also an early champion of naloxone, a lifesaving overdose reversal drug, and has worked to ensure that every first responder is equipped with the medication.
This report begins by providing context on the scope and impact of opioid misuse in the region and then lays out the basis of the city’s approach to addressing the epidemic. From there, the report outlines best practices for deploying local resources in response to an addiction crisis, organized around the lessons from Dayton’s experiences:
- Rapid and targeted data collection and use. In Dayton, detailed overdose data are collected and disseminated daily, weekly, and monthly to both ensure that those who overdose receive services quickly and to track emerging long-term trends. Overdose data broken down by jurisdiction and neighborhood also allow for tailored, targeted responses.
- Collaboration between agencies and organizations. In 2016, Montgomery County launched the Community Overdose Action Team (COAT), a partnership that broke down silos and fostered productive relationships between agencies. Agencies must be willing to step out of their traditional roles to identify assets and gaps, assign appropriate roles, and chart a collaborative path forward.
- A law enforcement strategy focused on prevention and support—not criminalization. In Dayton, law enforcement officers embraced an approach focused on supporting residents with substance use disorders. Collaboration across law enforcement agencies can also help reduce the supply of opiates, while taking legal action against pharmaceutical companies can help combat the stigma of addiction by publicly establishing the link between prescriptions opioids and substance misuse.
- Building a community of recovery and support. Creating a support system for people impacted by substance misuse reduces the stigma of addiction and helps individuals in active addiction enter and sustain recovery. People who are in recovery can provide valuable support, hope, and advocacy for individuals in active addiction.
- Access to treatment. Reducing the barriers to accessing treatment can help individuals take the first step toward recovery. Through proactive outreach, service providers can build long-term relationships with individuals in active addiction, provide information on available resources, and help connect them with treatment once they are ready to enter recovery.
- Promoting safer substance use. Expanding access to Narcan and sterile syringes can reduce the likelihood of overdose fatalities and the spread of disease, especially for those who are not yet ready to enter treatment.
There is still much work left to do in Dayton. But through the coordinated approach described in this report, the community has saved countless lives and made significant progress toward combatting the stigma of addiction. As cities nationwide consider their response to the opioid epidemic, local leaders should look to the model pioneered in Dayton.
Context on the epidemic
The city of Dayton is home to roughly 140,000 residents, making it the sixth largest city in the state.4 Located in Montgomery County, Dayton is a city known for manufacturing, innovation, and notable residents, Wilbur and Orville Wright. Like other midsized American cities, the decline in manufacturing jobs had a significant effect on Dayton’s economy over the past half-century, though economic health has improved in recent years.5 Today, Dayton’s top employers include Wright-Patterson Air Force Base, health networks, the education sector, and the county government.6
The region’s industry required hard work and labor, leaving many working-age and retired residents with chronic pain or unable to work. Prescription of opioids was a common response. Studies suggest that as many as 1 in 4 patients who are prescribed opioids for longer than a couple of weeks becomes addicted to those medications.7 In southwestern Ohio, many were left with an addiction.
Ohio developed a prescription opioid reporting system to address the growing problem of prescription drug misuse in 2006.8 In 2011, the state cracked down on pill mills, which the Centers for Disease Control and Prevention (CDC) define as for-profit clinics that prescribe painkillers to high volumes of patients who do not necessarily require painkillers medically.9 Subsequent to the state’s action, the number of opioids provided to Ohioans dropped by nearly 92 million doses in the three years from 2012 to 2015.10 However, the increased restrictions on prescription drugs unintentionally contributed to a new problem. Patients who could no longer afford or locate prescription opiates switched to a cheaper, more available alternative: heroin.11
Language choices
The language used to describe substance misuse can unintentionally perpetuate stigmas around addiction. Referring to people as “addicts” or a “substance abusers” suggests that those individuals are at fault for their disease. Instead, this report uses person-first language such as “individuals with substance use disorders” to reflect the understanding that addiction is a medical condition that can be addressed, and individuals should not be defined by their disease.12
Although heroin and other illicit drugs historically came to Dayton via bigger cities, Dayton became a so-called source city in the mid-2000s, meaning that drugs were supplied directly to Dayton and then distributed to other areas of the country.13 This direct supply led to an unprecedented rise in inexpensive, potent, and abundant heroin. And as a consequence, overdoses claimed more and more lives in Dayton, with the city’s northern and eastern neighborhoods most heavily impacted.
The Dayton Police Department (DPD) became aware of the magnitude of opioid use in the community around 2012, when a U.S. Department of Justice grant funded an analysis of crime in the eastern neighborhoods. Dayton police found that roughly 90 percent of solved property crime was related to opioid use.14
The introduction of fentanyl and fentanyl analogues had a devastating effect on the state of Ohio and city of Dayton. By 2016, Ohio was second in the nation for age-adjusted rate of deaths due to overdoses; drug overdoses had become the leading cause of death in the state for those younger than 55 years old; and fentanyl and fentanyl analogues were involved in 58 percent of overdose deaths in the state.15 Montgomery County was disproportionately impacted. From 2011 to 2016, it had the highest unintentional drug overdose rate in Ohio.16
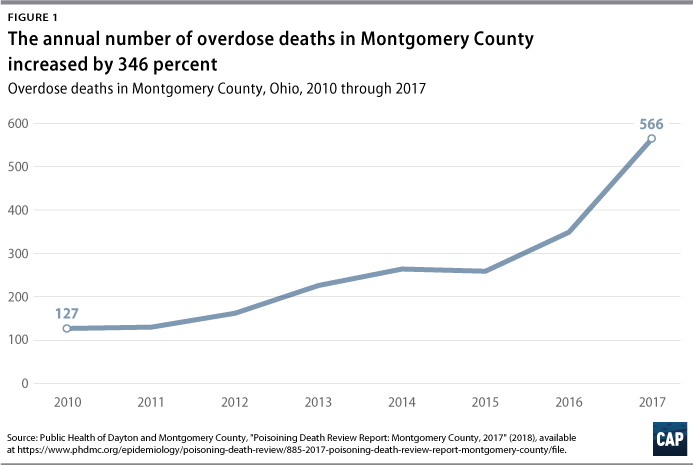
Unintentional drug overdose deaths in Montgomery County rose from 127 in 2010 to 566 in 2017. (see Figure 1) The rise in deaths corresponded to a rise in the presence of fentanyl and fentanyl analogues in overdose deaths. Not long ago, these drugs were almost unheard of. In 2015, fentanyl contributed to 41 percent of deaths, and heroin contributed to 45 percent of deaths. By 2017, fentanyl contributed to 64 percent of deaths, and heroin only contributed to 9 percent of deaths.17 Fentanyl and fentanyl analogues contributed to 85 percent of deaths in 2017.18
Fentanyl
Fentanyl is used typically only to treat cancer pain or other extreme pain. It is 50 times stronger than heroin and 100 times stronger than morphine. Across the United States, it was increasingly being mixed with heroin or other drugs, often without users’ knowledge.
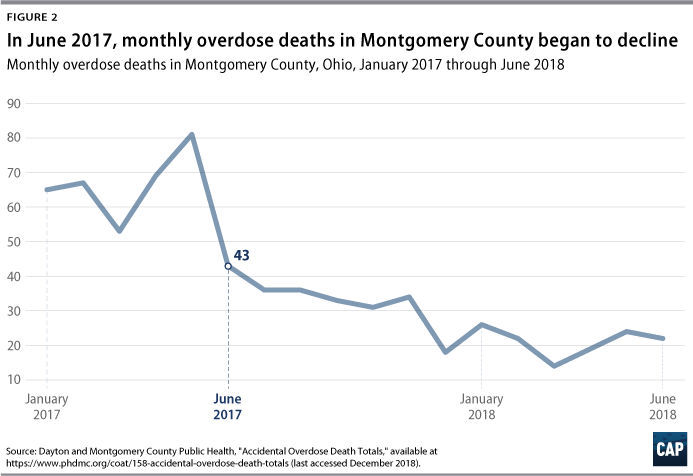
While deaths were at an unprecedented high throughout the first half of 2017, they later fell to levels comparable to those in 2015. (see Figure 2) This is a promising indication that the many resources being dedicated to the epidemic may be reducing the death rate.
Years of potential life lost
From 2010 to 2015, Montgomery County residents lost an estimated 26,278 years of life. Victims of drug overdose are, on average, far younger than those of the most common causes of death such as heart disease or cancer. The average overdose victim in Montgomery County was 41.5 years old—more than 30 years younger than the average victim of heart disease, at 75.6 years old.19 This means the potential collective impact of loss of life is far greater from death due to overdose. From 2014-2015, there were five times as many heart disease deaths as drug overdose deaths, yet years of potential life lost was 70 percent higher for drug overdose deaths.20 (see Figure 3) These early deaths will have a profound impact on the region for years to come.
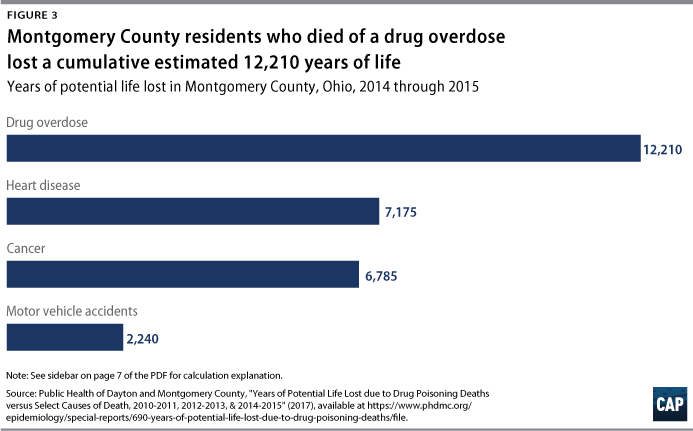
Years of potential life lost compares the average age of death for a particular cause with an estimated life expectancy of 65 years and multiplies this by number of deaths due to the cause. In Montgomery County, heart disease causes the highest number of deaths, followed by cancer. While deaths due to motor vehicle accidents are far lower, they tend to occur at younger ages.
Associated costs
Researchers at Ohio State University estimate addiction and overdose cost the state $6.6 billion to $8.8 billion each year.21 Costs to Dayton and the surrounding area have been accordingly high. From 2015 to 2018, the city of Dayton distributed more than $500,000 in Narcan, with the costs borne by a number of institutions. The cost of emergency response by first responders was around $340,000 in 2016. By 2017, that number rose to more than $610,000. In 2018, the cost was approximately half of the 2016 full year figure for the first six months of the year.22
Indirect costs are also high. For instance, data over 18 months in 2013 and 2014 showed around 90 percent of individuals interviewed regarding solved property crimes in Dayton’s East Patrol Division (EPOD) indicated that they had a drug issue.23 Finally, the rise in overdoses in surrounding areas means that Dayton is increasingly providing support to other jurisdictions. In the year ending May 30, 2017, the number of requests for overdose emergency from surrounding communities had risen to 2,323.24
Victim demographics
The average victim of an overdose death in Montgomery County involving opioids was a white man in his thirties. In 2017, nearly two-thirds of overdoses were of people aged 25 to 44. The majority of those deaths were males, while roughly one-third were females. (see Figure 4) More than 80 percent of those who died from overdoses were white.25
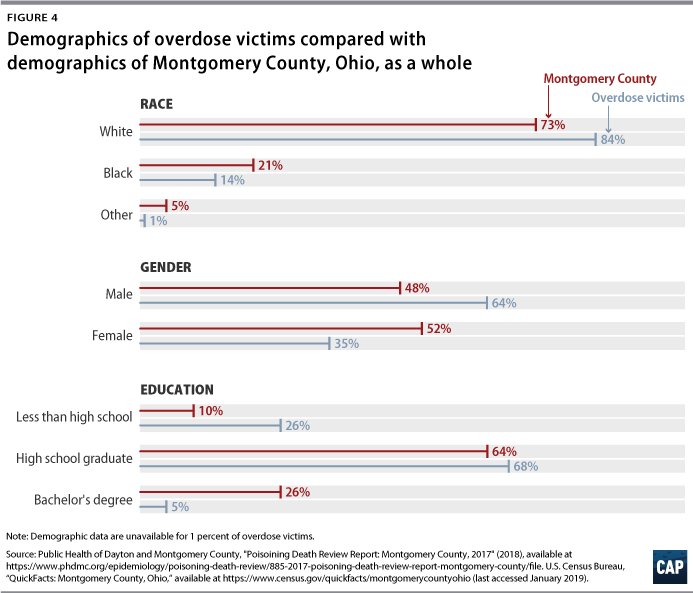
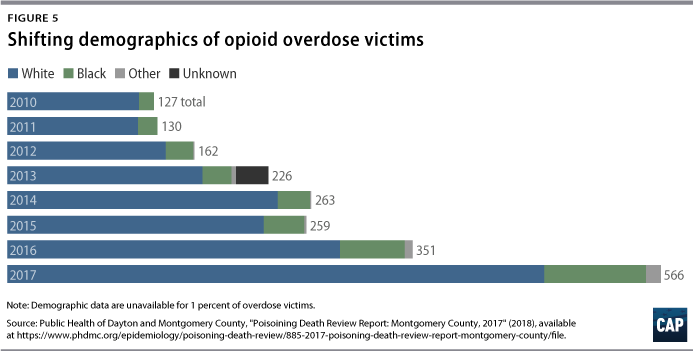
While the opioid epidemic has received attention as primarily affecting the white community, deaths among people of color have been rising at a disproportionate rate. According to the U.S. Census Bureau, 21 percent of Montgomery County’s population is black.26 By 2017, 16 percent of those who died of an overdose were black, up from 10 percent in 2010. (see Figure 5) However, nearly 98 percent of syringe service users in 2017 were white.27
This epidemic disproportionately affects individuals without a high school degree. This group composes only 10 percent of the population as a whole, yet represented 26 percent of deaths on average from 2010 through 2017.28 (see Figure 4)
As Dayton experienced a rising tide of addiction and overdose deaths, so did the rest of the nation. Across the country, 630,000 people died of drug overdoses from 1999 through 2016.29 The magnitude of deaths due to overdose shifted with the rise of opioid misuse. In 2016 alone, 42,000 Americans died from opioid overdoses.30 That year, age-adjusted rate of overdose death had more than tripled since 1999.31
Taking a new approach
In many ways, the unprecedented overdose death rate catalyzed action in Dayton. To save lives, the city would need to take a new approach to treating addiction. The realization that many addictions began with a prescription may have also contributed to an improved understanding that addiction requires a medical response—not a criminal justice system intervention.32 Unfortunately, previous substance misuse epidemics did not receive a similar response. Like many communities, Dayton was greatly affected by the crack epidemic of the 1980s. And like too many cities, Dayton’s primary response was increased law enforcement action, prosecution, and incarceration for impacted individuals, who were predominantly from communities of color. Nationwide, policymakers launched a war on drugs policy agenda that targeted black Americans and fueled the rise of mass incarceration.
In Dayton and beyond, policymakers have agreed that the war on drugs was a failed policy that must not be repeated. But the shift in the national conversation around addiction cannot be decoupled from the issue of race. Unlike the crack epidemic, which primarily affected communities of color, today’s opioid crisis exists predominantly among white Americans. In recognizing the disparate treatment of crack and opiates, policymakers must work to craft solutions that treat all addiction crisises as the diseases they are.
In Dayton, many individuals, agencies, and organizations began addressing the opioid crisis early on. They often did so independently, and throwing whatever they could at the problems they saw. This innovation and trial and error led to several successful grassroots programs. Many of those involved, however, ultimately realized greater collaboration was needed and that the barriers between jurisdictions must be removed. Today, the region’s response is coordinated among various agencies and local organizations. It is an approach that leverages data to fuel action. A common refrain is: “It’s not perfect, but we’re doing something.” That something is fueling a collective impact.
Key players in addressing the opioid crisis
Community Overdose Action Team (COAT)
- COAT: COAT is co-led by Public Health-Dayton & Montgomery County and Montgomery County ADAMHS. It consists of more than 100 community partnerships. Each organization described here provides individual services, but all have been organized under the COAT structure. COAT’s Backbone Support branch oversees its other branches, ensuring alignment and accountability.
City of Dayton
- Dayton Fire Department: Dayton Fire Department provides Narcan services. It also helps staff the Mobile Crisis Response Team.
- Dayton Police Department (DPD): The DPD helped initiate Getting Recovery Options Working (GROW) and Conversations for Change programs. The DPD also provides Narcan services. The Mobile Crisis Response Team is part of the DPD.
Montgomery County
- Montgomery County Alcohol, Drug Addiction, and Mental Health Services (ADAMHS): ADAMHS plans, funds, monitors, and evaluates publicly contracted services for persons with mental illness, alcohol, and other drug addictions. ADAMHS partners with around 40 service providers, and it also works in prevention and behavioral health. ADAMHS funds Narcan services and treatment services at the Montgomery County Jail. It co-leads the COAT.
- Montgomery County Sheriff’s Office: The Montgomery County Sheriff’s Office is part of multiple drug seizure task forces. It facilitates treatment services in the Montgomery County Jail and oversees GROW.
Health sector
- Public Health-Dayton & Montgomery County (Public Health): Public Health is an agency charged with improving the quality of life in the region through improved public health. Public Health co-leads the COAT, funds Narcan services, and directs the CarePoint syringe services program.
Nonprofit organizations
- East End Community Services: East End is a community-based nonprofit founded 20 years ago to meet the needs of East Dayton residents, focused on breaking the cycle of generational poverty and building a successful community. East End oversees Conversations for Change and Peers for Change and participates in GROW.
- Families of Addicts (FOA): FOA is a grassroots group that provides support and outreach to individuals suffering from substance use disorder and their families while focusing on reducing the stigma of addiction and recovery.
- Life Enrichment Center (LEC): The LEC is a faith-based nonprofit that provides services to residents of Dayton and surrounding areas. CarePoint syringe services are provided at the center, and Dayton’s FOA meetings are held here.
- Montgomery County Drug-Free Coalition: The Montgomery County Drug-Free Coalition is a collaborative partnership designed to promote a drug-free community through mobilizing stakeholders, educating the public, and advancing prevention efforts.
Private sector
- Cornerstone Project: Cornerstone is an outpatient treatment program with multiple locations and methods of service. Cornerstone also engages in community outreach, and one of its staff members directs GROW.
Dayton Police Department and East End Community Services partnership
At first, the opioid epidemic was largely invisible to authorities, in part due to a lack of data sharing across agencies. Then, in 2012, East End Community Services and the DPD received a Byrne Criminal Justice Innovation Grant from the U.S. Department of Justice to address high rates of property crime in East Dayton. (The Byrne Criminal Justice Innovation Program is now called the Community Based Crime Reduction Program.) It was not until the DPD began looking into the root causes of the property crime they were seeing that they realized much of the crime was committed to fund the purchase of opioids. The police department quickly recognized this was a growing problem, particularly on the east and north sides of Dayton. Moreover, police understood two things: First, that many of the perpetrators of these crimes were drug users who needed medical care and treatment; and second, that the issue of property crime would not be solved without first addressing addiction.
Not only did this partnership help uncover the scope of opioid misuse in Dayton, it also played a critical role in shaping the city’s response to the epidemic. East End, an organization that historically served as an advocate for low-income individuals, helped the police take a more community-centered approach that focused on treating substance misuse instead of criminalizing it. East End also helped bridge the gap between residents and the police, paving the way for more successful partnerships between officers and the community.
Early on in this partnership, the DPD began recording the names of people who had overdosed or exhibited risky substance use behaviors in a notebook—an improvised system for identifying individuals to connect to supportive services and treatment options. The ad hoc system later became a daily automated report on overdoses. By 2015, this list had roughly 1,000 names of individuals that the department would reach out to in order to offer support and connections to treatment.
At first, the partnership tried offering walk-in services for high-risk individuals, but they quickly found this model ineffective at attracting clients. They realized that they needed to take services directly to the community rather than expect residents to come to them. As a result, East End and the DPD launched Conversations for Change, a grassroots, community-based initiative that actively seeks out individuals who have overdosed to share information about paths to recovery.
The partnership between East End and the DPD also gave rise to Dayton’s Mobile Crisis Response Team and GROW blitzes, two initiatives that pair police officers with trained mental health professionals to conduct targeted outreach to individuals who have recently overdosed. These efforts began when a DPD officer heard about another Ohio county with several police officers whose full-time position was visiting the homes of community members who had overdosed to encourage them to seek treatment and supportive services. The Dayton officer thought this was a great idea, and although the department did not have budget capacity for such a project, the officer eventually visited a family following a fatal overdose. The officer expressed his sympathy to the victim’s father, who was moved that a police officer had visited his home to share his support. After the first visit, the officer reached out to his partners at the Cornerstone Project, East End, and FOA and said they must find a way to start visiting the homes of those who have been impacted by overdoses.
Key lessons learned: The DPD and East End partnership
- Instead of offering walk-in services, providers must bring interventions directly to people in need.
- Agencies should be willing to establish cross-sector partnerships and work outside of their traditional roles.
The partners began visiting people two hours per week. They found that people simply wanted to be heard and that they were often unaware of the resources available within the community. The people they visited were frequently surprised and moved that community members and law enforcement had come to their home trying to help them find treatment. Ultimately, most individuals visited were comfortable with the presence of a police officer.
The partnership’s efforts became the backbone of the city’s response to the epidemic. Both East End and the DPD continued seeing overdoses, deaths, and the impact of addiction up close. They remain partners and advocates in combatting the epidemic. The police department’s willingness to step out of traditional roles and into addiction support helped shift the DPD culture and inspire others to innovate.
Data collection and use
Data collection and usage across various agencies builds knowledge, informs decision-making, and enables more effective interventions. The following section offers insights for cities seeking to use data to guide local responses to the opioid epidemic based on the experiences in Dayton.
Understanding the problem: Tracking overdoses
Key lessons learned: Data
- Rapid, targeted data collection and disbursement fuels effective action.
- Overdose data broken down by jurisdiction and neighborhood allows tailored responses.
- The coroner’s comprehensive toxicology analysis provides important insight into drug usage trends.
- Compiling data across involved parties fosters collaboration and increases collective knowledge.
Today, agencies across Dayton collaborate to track data on the city’s overdoses. Each day, the DPD’s Mobile Crisis Response Team receives a detailed report on all city overdoses, including a photo of the victim; the number of overdoses that person has had since April of 2017; the location of the most recent overdose; the amount of Narcan administered; and the individual’s address. The DPD also has a protocol for flagging arrests, field interviews, and crime reports with connections to opioid misuse. These reports provide the vital information the team needs to follow up with overdose victims to offer information on treatment and other supportive services. The GROW team leverages similar overdose reports from participating jurisdictions.
Working in partnership, Dayton police and fire departments compile a monthly report on overdoses in the city. This report totals information and breaks down data by neighborhood. The data include counts of the number of fatal and nonfatal overdoses, arrests, and milligrams of Narcan administered. Year-to-date counts are also provided. This report provides ongoing updates on trends within neighborhoods and across the city. (see Tables 1A and 1B for a sample report)
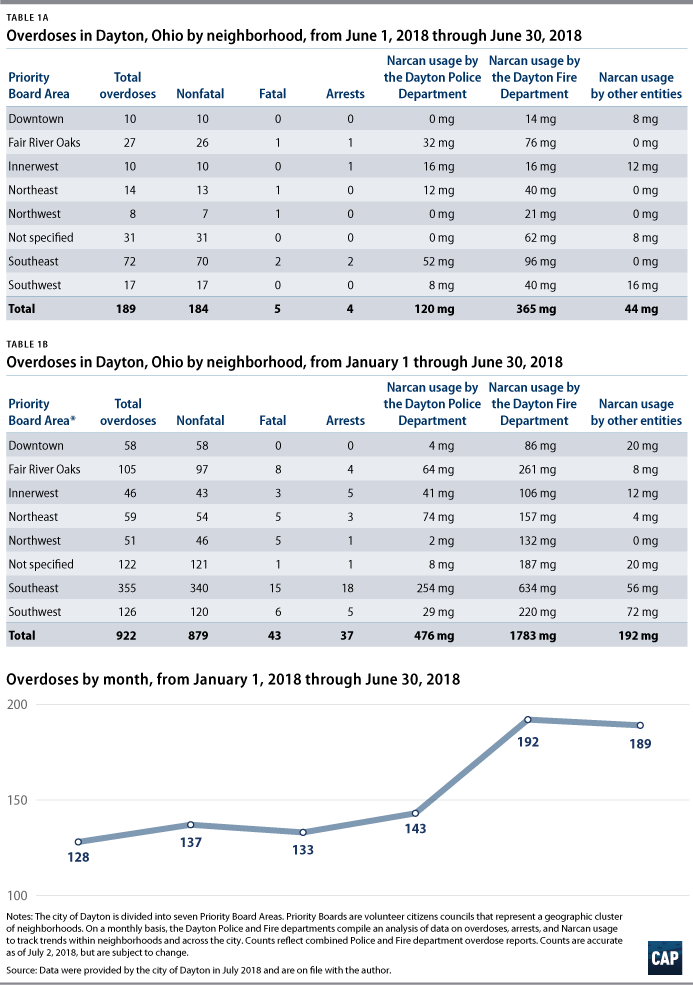
The Dayton Fire Department has collected and compiled comprehensive data on overdoses requiring Narcan since 2013. This data slicer allows counts and comparisons by various markers, including neighborhood, day of the week, month, year, sex, and race. The slicer can be used for in-depth analysis, including assessment of seasonal trends.
Naloxone
Naloxone, sold under the brandname Narcan, is a lifesaving medication that rapidly reverses the symptoms of an opioid overdose. Naloxone works by binding to the opioid receptors in the brain and blocking the effects of the overdose, restoring the individual’s ability to breathe normally.33
The Montgomery County Coroner’s office publicly shares weekly updates on the number of overdose deaths in the county. The data are updated each Friday on Public Health’s website and synced to the coroner’s website. It includes provisional counts of deaths, breakdowns by jurisdiction, and historical data. The jurisdictional itemization allows law enforcement to intervene more intentionally if they see increasing deaths in a particular area. Such updates used to take a year to be finalized and shared. The frequent updates permit quicker, more appropriate responses. The provisional data are typically nearly correct. The end of 2017 report counted 562 deaths, and the final number only increased by four deaths.
Mapping the epidemic
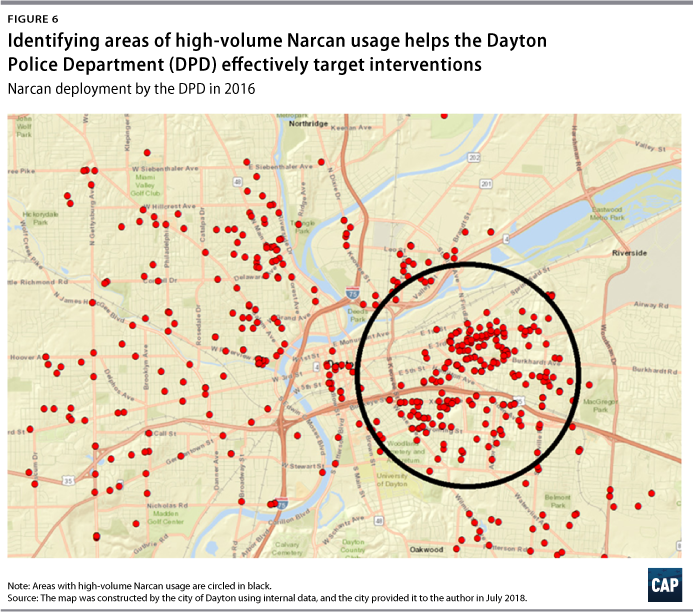
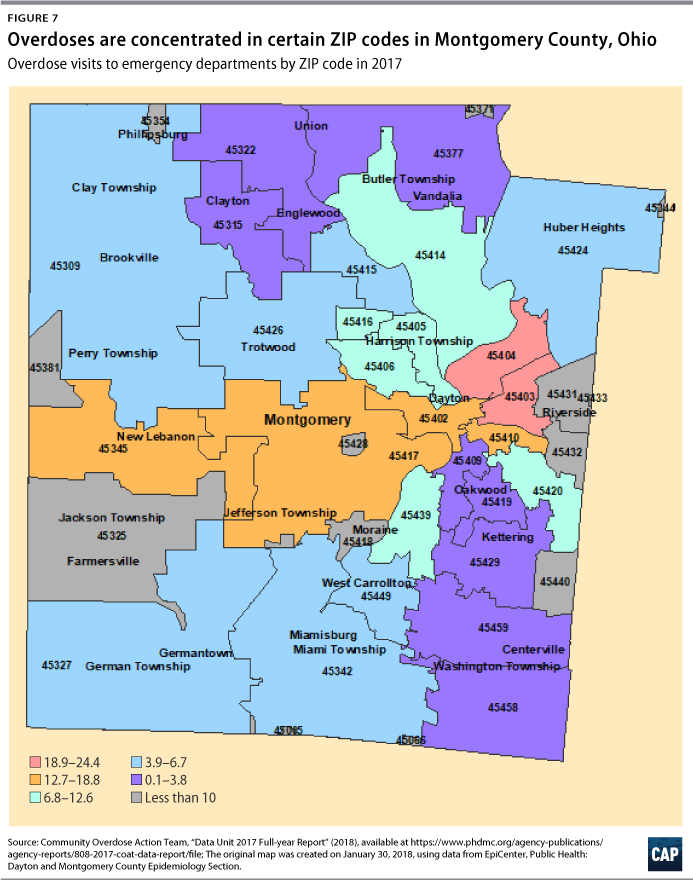
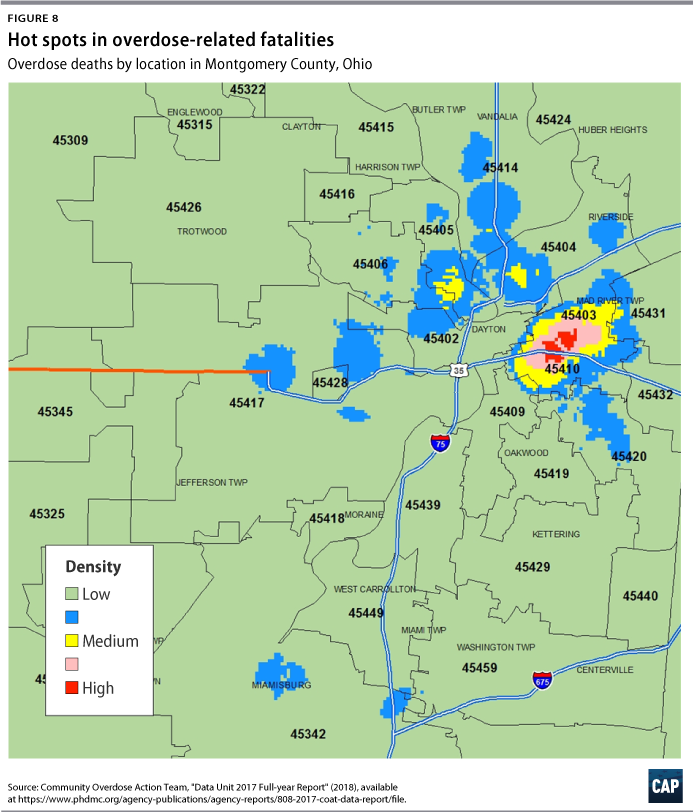
To effectively target interventions, jurisdictions must understand the geographic concentration of opioid misuse and overdoses. The DPD creates visual maps of overdoses and opioid-related crime to identify hot spots and target areas for interventions. Through year-to-year comparisons, the DPD is also able to assess changing patterns in opioid use. Figure 6 shows a sample map depicting DPD’s 2016 Narcan use and highlights high-volume use in the city’s eastern neighborhoods. County-level density maps of overdose emergency department visits by ZIP code and heat maps of overdose deaths serve a similar purpose. (see Figures 7 and 8)
Identifying trends in drug usage
When the data on drug usage are incomplete, it can be challenging for local leaders to identify trends and effectively meet the needs of the community. To help fill gaps in knowledge, CarePoint developed a new patient survey that collects information on the client’s drug of choice, number of overdoses experienced, cause of overdose, and any previously diagnosed mental health disorders. The program also counts visits, referrals made to treatment, and other services provided. This information can be leveraged in improving continuums of care and developing increasingly targeted interventions.
Another challenge arises from toxicology analyses, which are often incomplete. Across the country, fentanyl analogues are not commonly tested for, and some are difficult to detect.34 But knowing which ones are driving overdose fatalities provides valuable insight into drug use, production, and trafficking patterns. This in turn aids law enforcement, treatment, and intervention efforts. To address this shortcoming, the Montgomery County coroner now tests for many compounds, including around 30 variations of fentanyl analogues. Tests for fentanyl were originally completed only when it was mentioned in the individual’s personal history; however, the coroner began routine testing for fentanyl around 2013 and for fentanyl analogues in 2016.35
The COAT data report
The Community Overdose Action Team (COAT), which is discussed in greater detail below, formed its data unit with a commitment to taking data-driven action. COAT began by identifying the data points that its branches would need to support operations as well as the information that would be useful for the community to have. The data team includes individuals from Public Health, Wright State University, the DPD, Montgomery County, the Greater Dayton Area Hospital Association, the Montgomery County Coroner’s Office, the Montgomery County Sheriff’s Office, Montgomery County ADAMHS, and the University of Dayton. These partners collect and compile data for the COAT branches’ use and to share with the public. In 2017, the group released its first annual data report, which was the first report to compile the vast amounts of data that participating agencies collected. Moving forward, a similar report will be shared every six months, helping to inform collective action.
The path forward
In 2014, Public Health developed a strategic plan for meeting residents’ health and wellness needs. Known as the Community Health Improvement Plan (CHIP), the effort ultimately catalyzed coordinated action through an interagency collaborative.
One of the plan’s three priorities was improving behavioral health outcomes. But when Public Health began implementation in 2016, the agency realized that it had little data to illuminate the community’s behavioral health needs and existing gaps in service. Anecdotally, public health officials heard many promising ideas around how to provide mental health and addiction support, but they lacked sufficient evidence to inform decisions. The agency accordingly commissioned a behavioral health needs, gaps, and systems barriers analysis to guide future decision-making.
The final report, released in May 2018, includes both quantitative and qualitative analysis to provide a comprehensive description of the behavioral health landscape. Importantly, researchers conducted focus groups and interviews to capture the experiences and insights of clients, providers, and other key stakeholders. Of course, many policies and initiatives were implemented based on what was already known or guessed while the report was in progress. That said, the report’s insights will guide and inform decisions moving forward.
Collective impact: The Community Overdose Action Team
As the magnitude of overdose fatalities in Dayton and Montgomery County grew, more and more agencies and organizations became involved in addressing the crisis. Prior to 2016, however, groups were working in silos to address the crisis with little coordination.
Recognizing the need for collaboration, in 2016, the Montgomery County commissioners convened a meeting of city and county partners with jurisdiction over various areas relating to substance misuse. Initial group meetings were contentious with a great deal of finger-pointing. In August 2016, the commissioners hired a consultant to train the participating entities on the principles of collective impact. This training was the beginning of figuring out how to work together.
The group learned that individuals and entities must leave their typical roles and operational procedures at the door and identify the strengths and resources they could bring to the table. Learning to overcome those barriers was the greatest lesson of collaboration and became the foundation for ingenuity. The training also instilled the importance of group buy-in: Everyone had to be ready to partner before the collaboration could truly take off.
Key lessons learned: COAT
- Collective impact training provides helpful guidance for crisis response.
- Agencies and organizations must be willing to drop their traditional charges.
- Only then can they collaborate to identify assets and gaps, chart a path forward, and assign appropriate roles.
- Accountability and communication structures are the backbone of collective action.
- COAT’s model provides a blueprint for future crisis response.
On a logistical level, partners learned that successful interagency initiatives must be co-led by those who have statutory jurisdiction in the area. Those groups must be committed to their co-ownership, and they must understand the roles and responsibilities of each entity.
The partners presented their collaboration plan to the community in September 2016. To build COAT, they leveraged a strategy known as the Incident Command System, an approach to emergency management focused on helping agencies work together effectively.36 This structure was chosen for several reasons: 1) It is designed for emergency response; 2) Public Health and Montgomery County first responders were already familiar with this system; and 3) It provided a model for integrating systems and resources, ensuring alignment, and providing accountability.37 Notably, the county leveraged an emergency response system more than one year before the president declared a national public health emergency.
COAT has a Backbone Support group that oversees the various branches, ensuring alignment and collaboration. Eight branches target particular areas of need also identified as national and state priorities. The branch titles and charges are as follows:
- Prevention: Prevent opioid and illicit drug misuse
- Treatment and Recovery: Expand access to treatment and community supports
- Illegal Opioid Supply Control: Decrease the supply of illegal opioids and other illicit drugs
- Response: Develop emergency plans to respond to individuals in crisis or a large casualty event
- Harm Reduction: Increase capacity for harm reduction efforts, including syringe services and Narcan distribution
- Prescription Opioids: Promote the use of best practices for opioid prescribing; raise awareness and knowledge about the dangers of opioids
- Criminal Justice Services: Expand access to treatment options for those involved in the criminal justice system
- Education and Information: Raise public awareness and knowledge about the use and misuse of opioids38
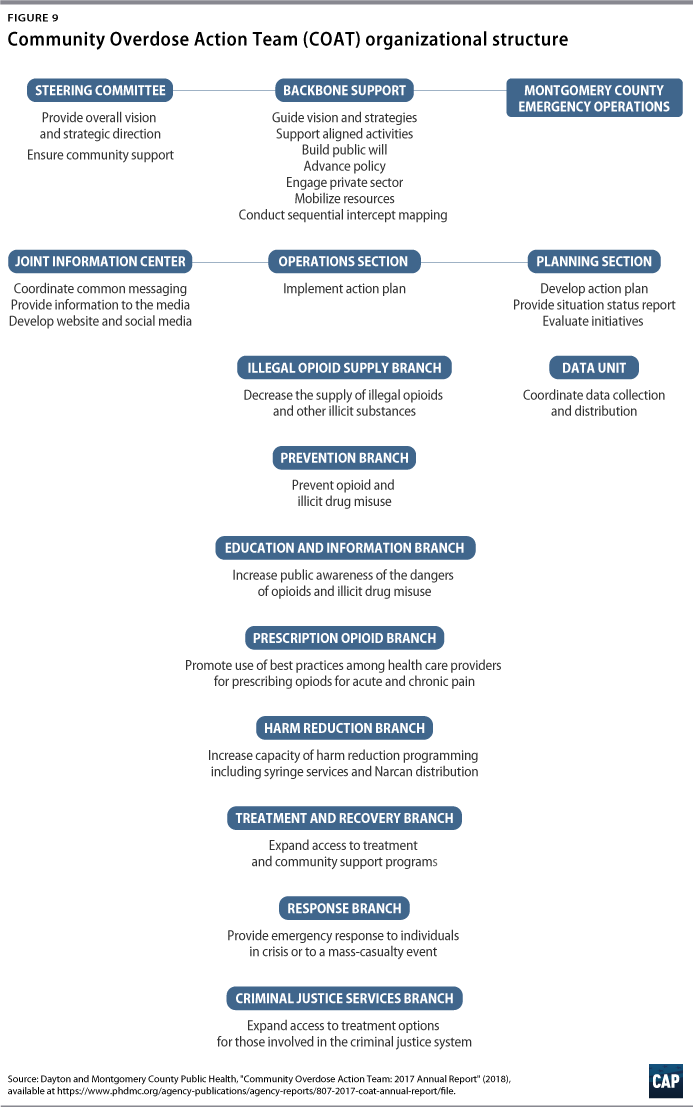
In the first year and a half of COAT’s operation, each branch created 30-day operational plans. By 2018, COAT moved to a long-term planning phase, and branches now develop 60-day operational plans.
Learning from the experiences of other communities proved valuable to COAT. The Response branch, for example, took note that both Cincinnati, Ohio, and Huntington, West Virginia, had experienced 24-hour periods with unusally high levels of overdoses. Recognizing the possibility for a similar occurence in Montgomery County, the team built a protocol for how to respond in the event of a rapid rise in overdoses in a concentrated period of time. This protocol included commitments from other communities that would join forces with Montgomery County to respond to such a crisis if needed.
The collective impact model effectively broke down silos and fostered relationships between agencies. For instance, COAT enabled meetings between the Dayton city commissioners and the Board of County Commissioners as well as between the Board of Health and ADAMHS. These groups did not previously have systems for working together in this context. And while they were experienced in coordinating actions in a variety of areas, they typically did not respond to large-scale public health emergencies that would require more open and flexible collaboration and communication.
The model ensured accountability to one another and to the community, as both internal and external communication increased rapidly. Moreover, the implementation of an emergency-response structure caused the community and involved partners to fully internalize the opioid epidemic as a priority area and public emergency.
COAT’s experiences yielded valuable insights into the importance of coordinating communications strategies to ensure alignment across the group. Consistency in communications with the public is a difficult but necessary component of collective action. In early 2017, COAT did not provide a united message as death numbers spiked, with various agencies offering different opinions about what was happening. To ensure a more consistent response, COAT established a Joint Information Center to coordinate messaging across partner groups and provide regular briefings to the media. Partners also notify one another when media representatives or the public request information to ensure response alignment. COAT has also found that sharing data among the group can help partners develop a common understanding of the problem and speak from the same page.
Monthly overdose deaths were lower in the year ending June 2018 compared with the first half of 2017. While it is difficult to determine a precise cause for such declines, it should be noted that COAT made significant contributions to service provision during this period. In 2017, COAT was responsible for developing or enhancing 45 services, from strengthening treatment options and continuums of care to expanding outreach to people in active addiction. COAT leverages the contributions of more than 100 community partnerships and more than 200 individuals, including family members of individuals with opioid use disorder, individuals in recovery, and other concerned residents. People who wish to help are not turned away.
Perhaps most importantly, the COAT model provides a blueprint for early action in any future crises. Even as opioid-related fatalities decline, the county is seeing an increase in methamphetamine use, presence, and overdoses. With a structure for collaboration in place, the agencies that comprise COAT are prepared to take collective action—regardless of the primary drug of choice. The partnership has allowed for a proactive approach to seeking funding, as well. Initially, COAT members had to reallocate organization resources to fund the emergency response. But because COAT has identified resource gaps across priority areas, it can now proactively respond to available funding opportunities, coordinate requests in advance, and ensure alignment on which entities will take the lead.
Case study: Prescription Opioid Branch
COAT’s Prescription Opioid Branch is charged with promoting the use of best practices for opioid prescribing and raising awareness about the dangers of opioids. Its regular members include representatives from Public Health, physicians from local hospitals, and substance use treatment providers.
This branch had three key successes in 2017:
- Supporting the development of an addiction curriculum at Wright State University’s Boonshoft School of Medicine to train doctors and medical students in the treatment of opioid use disorders
- Working with Wright State University’s Boonshoft School of Medicine to offer training for prescribers on the Screening, Brief Intervention and Referral to Treatment (SBIRT) model, an early intervention strategy that identifies patients engaging in risky substance use behaviors and offers targeted interventions to prevent addiction39
- Developing PAUSE, a pathway for physicians and pharmacists to help patients manage chronic or benign pain through alternatives to opioids
The Prescription Opioid Branch’s 60-day operational plan describes five ongoing actions and four planned actions alongside their estimated completion dates. Key current actions include partnering with Wright State University to incorporate SBIRT into its medical residency program and researching opioid prevention videos to be used in doctors’ offices.
In a typical meeting, subcommittees report out on their progress, members share relevant information or updates, and the group works on a collaborative project. In the June 2018 meeting, for example, members shared updates on 10,000 drug disposal bags that were deployed to various hospitals and agencies. Public Health discussed a strategy for preventing an imminent outbreak of hepatitis A, describing both the high-risk population and proactive steps that would be taken to address the outbreak. Practitioners were then able to share best practices and information with one another and could take information back to their respective agencies. Finally, the group collaborated on planning a seminar to educate clinicians on serving individuals with substance use disorders and on alternatives to opioid treatment.
Law enforcement: Interdiction, intervention, and more
Dayton’s approach to the opioid crisis is rooted in the understanding that addiction is a disease, not a crime. However, a comprehensive effort to address the opioid epidemic must also include law enforcement actions to reduce the availability of illegal substances—while ensuring that individuals with substance use disorders are not criminalized.
The city of Dayton, Montgomery County, and other jurisdictions across the Miami Valley region of southwestern Ohio—where Dayton is located—collaborate on a number of initiatives aimed at making illegal substances not readily available. In 2017, the DPD seized more than 22,000 grams of fentanyl and 13,000 grams of heroin.40
Key lessons learned: Drug seizures
- Collaboration across jurisdictions is necessary to effectively respond to drug trafficking.
- Law enforcement should be prepared to provide connection to treatment when conducting blitzes.
The Regional Agencies Narcotics and Gun Enforcement (R.A.N.G.E.) Task Force consists of 12 law enforcement agencies at the local, state, and federal levels. The Task Force’s enforcement activities are specifically targeted at disrupting the distribution of illegal drugs in Montgomery County and nearby Clark County. In 2017, R.A.N.G.E. collected 63 firearms and seized currency and illegal drugs valued at nearly $9 million, including more than 9,000 grams of heroin and fentanyl.41
The Miami Valley Bulk Smuggling Task Force was formed as a response to the Miami Valley region’s genesis as a so-called source city—a U.S. locale that serves as a hub for transporting illegal drugs throughout the country. This task force consists of nine agencies that target major drug cartels sourcing high amounts of drugs to the Dayton area. Their work includes conducting longer investigations as well as monitoring and communicating with area hotels. The task force focuses both on collecting drugs and seizing money to prevent it from reaching cartel leaders. Responses to tips and investigations must therefore be rapid. In 2017, the task force seized more than 33,000 grams of fentanyl, compared with just more than 1,000 in 2016.42
The Montgomery County Drug-Free Coalition conducted seven law enforcement blitzes in 2017. Importantly, these blitzes are more than simply apprehending people who are distributing illegal drugs; they are also an opportunity for law enforcement to connect people in active addiction with Cornerstone Front Door—a conduit between law enforcement and treatment facilities—along with educating the community on the dangers of opiates.
Prescription opioid lawsuit
On June 5, 2017, the city of Dayton filed a lawsuit against pharmaceutical companies, distributors, and physicians it charged with causing or contributing to the opioid epidemic. Dayton was one of the first of many cities and states to file suit. The suit fundamentally argues that the companies misled physicians and the public about the risk of addiction and the effectiveness of their medications. The physicians named contributed to normalizing the use of opioids to treat pain.43
Through the lawsuit, Dayton takes two important steps. First, it combats the stigma around drug use and the belief that addiction is a moral failing. It does so by publicly naming the link between prescription opioids and the use of illicit opioids like heroin and fentanyl analogues. Studies suggest that nearly 80 percent of people who inject heroin first used prescription opioids.44 Vocalizing the link between trusted doctors and addiction to opioids helps the public understand that addiction is a disease that can happen to anyone. Second, the city seeks to recoup the money it has spent on efforts to solve the opioid crisis. Since 2015, more than $500,000 has been spent on Narcan alone, and the city of Dayton has spent more than $1.3 million on responding to overdose calls.45 This does not include costs borne by the public for treatment, recovery, lost productivity, or other interventions.
Building a community of recovery and support
Many in Dayton recognize the importance of community in supporting individuals beyond acute treatment and through recovery. While much must still be done to improve the continuum of care, Dayton’s recovery community is growing in numbers and strength. The nonprofit group Families of Addicts (FOA) has worked for several years to connect families, individuals in active addiction, and individuals in recovery to services and to one another. Various interventions also leverage peer recovery specialists, who serve as voices of hope and understanding for those in active addiction. Finally, there is ongoing conversation around providing employment and housing support to people in recovery.
Families of Addicts
FOA is a nonprofit organization that supports people affected by addiction, offers connections to services, and advocates for additional investments for addiction resources. FOA is led by volunteers seeking to build a community of individuals affected by addiction and reduce the stigma around addiction.
Lori Erion founded FOA in the fall of 2013 with a small meeting of people gathered to talk about addiction. Erion is in recovery herself and was inspired to found the group after she began learning from her daughter about her heroin addiction. Today, the organization exists in five Ohio counties with groups in other states attempting to replicate the program.46
Anyone touched by addiction is welcome to attend weekly meetings, which often feature open discussion and educational speakers or videos. Meetings in Dayton regularly draw around 100 participants, including peer supporters, people in recovery, people in active addiction, people hoping to enter recovery, and family and friends.47 In 2017, weekly attendance totaled more than 7,500 individuals.48
Every meeting includes milestone celebrations, a time for anyone to share progress or something they are proud of, no matter how small. Those who relapse are not shamed; rather, relapse is recognized as part of the disease. The thinking is that the time in recovery someone built up before relapsing is not lost and should still be honored.
The culture of support and acceptance aids FOA in developing a trusting community. As a result, the group provides a surrogate family for those who have lost or strained ties with loved ones due to their addiction.49 Experiencing one’s own or a loved one’s addiction can be an incredibly isolating experience, so this community can serve as an essential support system. People in Dayton often comment on the group’s loving, welcoming, and warm environment.
FOA also plays an important role for individuals in long-term recovery. These inviduals say they feel valued, and they contribute to the community by educating others and providing a model of hope to those newly in recovery.50 Families, in turn, gain understanding of addiction and recovery and are offered hope for their loved ones.
Importantly, open discussions around addiction help eliminate the stigma families and people in active addiction face. The traditional element of anonymity advocated by 12-step programs contributes to a lack of awareness around the number of people living in recovery. Therefore, FOA believes that educating the public and those in active addiction around the vast number of people living in recovery provides hope and decreases stigma.
Key lessons learned: FOA
- The anonymity of addiction and recovery contributes to stigma.
- Models of hope help people in active addiction enter recovery.
- Sustained recovery requires a community.
- Relapse is not a moral failing or the end to recovery; it is part of the disease.
FOA participants learn a new language to describe their recovery. Specifically, this language advocates that people in recovery should dispense with the common introductions of “I am an addict” or “I am an alcoholic.” Instead, many participants say, “I am a person in long-term recovery,” before explaining what that means to them.
In addition to the regular meetings, FOA hosts events intended to foster understanding and education within the community. Two events, Rally4Recovery and Families of Addicts Help Summit: The Secret Affecting Your Bottom Line, are important examples of the type of activism FOA practices.
The annual Rally4Recovery is focused on fighting the stigma around mental health disorders and addiction by celebrating individuals in recovery and bringing together loved ones and community members. In addition to educating the community around addiction, Rally4Recovery serves as a beacon of hope for individuals in active addiction and their families by demonstrating the number of people living in recovery and the existing community of support.
FOA also sponsored an event for local business and civic leaders, called the Families of Addicts Help Summit: The Secret Affecting Your Bottom Line. The convening, which featured speakers and a screening of a film about the stigma of addiction, focused on helping employers support their employees who are affected by a loved one’s addiction. Employers learned how an individual’s addiction can affect an entire family and in turn create ripple effects in the workplace. For example, many family members report that they are sometimes distracted in the workplace due to worries about their loved ones’ struggles with addiction. By connecting employees with FOA’s support network, employers are able to both support their employees’ well-being and improve workplace performance.
Beyond official events, FOA is a constant support to others and shares treatment resources with anyone who asks for help.51 In 2017, the organization made more than 450 calls to support people affected by addiction, and it connected 200 people to treatment.52
Certified peer supporters
Peer supporters are individuals in long-term recovery who offer support and guidance to individuals in active addiction. Several organizations and initiatives leverage volunteer peer supporters or staff certified peer supporters to enhance their work.
Peer supporters also help those who have never experienced addiction themselves better understand addiction and recovery. Most importantly, they serve as models of hope and more deeply identify with those in active addiction. While individuals who have not been through addiction themselves have compassion, they have not experienced the treatment process themselves. Peer supporters can therefore have an outsized impact on people in active addiction because they have walked a similar path but have moved into recovery.
Key lessons learned: Peer support
- Individuals in recovery have an essential and uniquely impactful voice in helping others enter treatment.
- Serving as peer supporters provides an important role for people in recovery.
- At times, peers who are one or two years into recovery can be more effective than those in longer-term recovery in reaching those in active addiction.
- A number of grants provide funding for full-time peer supporters.
East End Community Services, FOA, GROW, the Mobile Crisis Response Team, the Montgomery County Jail, and Conversations for Change all benefit from peer supporters in various ways. (see details below) Many COAT branches include people in recovery.
East End’s Peers for Change program staffs two full-time certified peer supporters who encourage and advise individuals in active addiction and treatment. East End originally partnered with peer volunteers before securing funding for full-time positions through a grant from the Office of National Drug Control Policy.
The Peers for Change focus on following up with individuals who proactively seek help or who have overdosed. Peers for Change staff visit people held at the Montgomery County Jail to help link them to treatment as they are preparing to be released. Peers for Change staff also participate in Conversations for Change and GROW, and they often ride with the Mobile Crisis Response Team. A licensed social worker partners with the peer supporters to provide case management to clients.
Peers for Change is a new program, so data on its success are limited but promising. From March 2018 through May 2018, the peer supporters and social workers engaged with 23 clients and nine family members or friends and helped seven individuals access treatment.53
Voices Project by Indigo Life Media
Voices Project seeks to elevate the stories of people in recovery and their loved ones through brief video segments. The project currently consists of 14 videos of Dayton area residents telling their stories of addiction and personal paths to recovery.
People in recovery help fight the stigma around addiction by sharing their stories and speaking out publicly. This can be healing and empowering for participants. Family members discuss their paths to understanding and compassion for their loved ones suffering from addiction. The video format allows wide sharing and easy access. And it serves to educate the public and increase awareness around addiction and recovery. Finally, it is another means of offering hope to those fighting active addiction and for their loved ones.54
Access to treatment
It is difficult to estimate the number of individuals in the Dayton area who have an opioid use disorder, who are in need of treatment, or who are receiving treatment. There are currently 792 residential treatment beds available in the Dayton area, and treatment capacity has increased in recent years.55 Most leaders agree that access to medication-assisted treatment has also improved.
However, state and national numbers still suggest that available treatment sources are not enough. Researchers at Ohio State University estimate somewhere between 92,000 and 170,000 Ohioans were addicted to opioids in 2015. They also estimated that, at that time, the state could only meet 20 percent to 40 percent of the need for treatment. This estimate reflects the best case scenario, so the true capacity could be lower.56
Nationally, estimates suggest that only around 10 percent of people who need treatment are receiving it. The process for entering treatment can be incredibly difficult. Successfully receiving treatment often requires navigating complicated insurance requirements, being aware of and selecting one of the various treatment pathways, and finding a bed. This can take time, paperwork, and many phone calls.
Medicaid expansion has likely afforded many Dayton residents access to necessary treatment. Ohio’s implementation of the Medicaid expansion brought coverage to individuals up to 138 percent of the Federal Poverty Level in 2014.57 As a result, more than 700,000 Ohioans enrolled in Medicaid.58 Evidence suggests the Medicaid expansion led to increased treatment of opioid use disorder throughout the country.59 Medicaid recipients are twice as likely to receive treatment as those with private insurance or without insurance.60
Several of the initiatives discussed below originated from a partnership, described above, between the DPD and East End, an organization that historically served as an advocate for low-income individuals in East Dayton. The partnership, forged as part of the Byrne Criminal Justice Innovation grant, helped the police take a more community-centered approach to addressing substance misuse and helped bridge the gap between community members and the police. Importantly, the partnership helped the DPD step out of their traditional enforcement-focused role to help connect residents struggling with addiction to treatment. In turn, the police department’s willingness to move toward a focus on addiction support helped shift the culture and inspire others to innovate.
Conversations for Change
After an analysis of property crime revealed the magnitude of opioid misuse in Dayton, the DPD began offering walk-in services for individuals seeking treatment. When the walk-in model failed to attract participants, officers recognized that they needed to take services directly to the community. Soon after, the department leveraged its partnership with East End to launch Conversations for Change, an initiative that seeks out individuals struggling with addiction and invites them to join a supportive community meeting where they can learn about available services and paths to recovery.
Since its launch in 2014, Conversations for Change has been recognized by Michael Botticelli, the former director of the White House Office of National Drug Control Policy, as a strong example of law enforcement supporting recovery efforts.61
Events are approximately two hours long and include a meal for participants. Participants who stay for the entirety of the event receive a grocery store gift card. There are four stages to the conversations, and attendees may be divided into groups and participate in the stages in different orders.
Stage one: An impact panel provides treatment resources and access to peer recovery supporters. Specifically, a clinician provides an overview of treatment options and the many paths to recovery in the region. The clinician also delivers addiction education and works to destigmatize the illness. This is important for families as well as individuals in active addiction who have internalized the stigma and may be experiencing shame and self-judgment. Participants have the opportunity to meet with various treatment providers afterward.
Stage two: Attendees participate in a community resource panel. Conversations for Change now has more than 30 multisector partnerships with service providers, who may provide resources such as Medicaid enrollment assistance, employment services, and connections to housing. Some Conversations for Change events primarily focus on offering resources for employment and are attended by local employers. All providers who attend Conversations for Change must commit to serving clients in a timely manner that puts clients’ needs first. Partners who do not abide by these expectations are asked to leave. People in active addiction seeking help may need a variety of social services that are not typically housed in one place, which often requires many individual visits or phone calls to secure all necessary services. East End’s expectations push providers to ease clients’ burden by quickly providing services all in one place.
Stage three: A facilitator trained in transformative mediation or motivational interviewing leads a one-on-one conversation. This stage encourages the identification of a personal path to recovery. It is a nondirective and nonjudgmental process designed to ensure individuals do not feel alone or judged. Guided dialogue with an experienced mediator allows individuals to articulate why they may wish to stop actively using opioids. By responding to verbal and nonverbal cues through questioning, the mediator seeks to help the individual overcome fears around entering treatment while keeping the conversation client-centered and client-led. Individuals can then discuss their ideas and plans for their path to recovery, leveraging insights gained from the earlier education portion. Throughout the conversation, mediators summarize and recap to develop clarity around next steps the client wishes to take.62
Stage four: Attendees participate in a conversation focused on overdose education and prevention. Participants are taught to recognize the signs of an overdose and are trained in CPR and to administer Narcan. Narcan is provided through Project DAWN.
Several key lessons have emerged from Dayton’s experience with Conversations for Change. Early on, organizers learned the importance of establishing a safe space for participants—even before the event begins. The first meetings were sparsely attended, in part because the invitations were mailed from the DPD. With the police department listed as the return address, individuals were wary of attending. Only three individuals attended the first meeting, and only one joined the second meeting. After that false start, East End was listed as the return address on mailed invitations, and all events were held in strategic, community locations, convenient for those in targeted areas. Organizers also hand-deliver invitations to individuals who have overdosed and share information broadly in communities where addiction is most heavily concentrated, encouraging participation from people in active addiction along with their family and friends.
Key lessons learned: Conversations for Change
- Law enforcement agencies should be willing to work outside of their traditional roles.
- A safe space is required. This means that law enforcement officers should be in plainclothes, and media should not be permitted.
- Targeted, proactive invitations must be sent to achieve desired attendance. Walk-in events are less effective.
- Harm reduction services can reach those not yet ready for treatment.
- Convening treatment and social services in one location eases the administrative burden many people face.
The DPD remains a key partner in the event, although officers must attend in plainclothes to foster a safe space. Initially, some thought that a lack of visible police presence might lead to crime at the event, but that concern has been proven unfounded. To ensure a safe space, no media outlets are permitted to join the event.
Dayton’s experiences have also helped identify the most effective messengers of hope and motivation for individuals in active addiction. At the end of a Conversations for Change event, the full group reconvenes to hear a personal story of recovery. FOA has found that having peers who are one or two years in recovery was more effective than those in longer-term recovery. If someone is 10 years into their recovery, it can feel less attainable to those in active addiction.
Conversations for Change has had success reaching individuals impacted by addiction. Originally, organizers believed participants attended because of the gift card. However, an evaluation of Conversations for Change suggested that people attend the events because they were seeking community. From May 2014 to May 2018, 22 events were held, 705 people attended seeking services for themselves or a loved one, and 618 participants received Narcan training and a Narcan kit.63
GROW: Getting Recovery Options Working
Started in 2016, GROW is an outreach initiative that goes directly to those in need in nine jurisdictions throughout the county. It is overseen by the Montgomery County Sheriff’s Office and directed by a Cornerstone staff member.
Every two weeks, staff and volunteers meet to conduct a blitz, where teams of volunteers visit high-risk individuals and neighborhoods. On a targeted blitz, participants visit the homes of those who have overdosed in a particular jurisdiction in the past week. On other blitzes, they go door to door in neighborhoods with high drug use. In both cases, organizers offer to share information on treatment options. To identify target areas for disseminating treatment information, organizers leverage overdose reports or other data that local law enforcement provides.
Key lessons learned: GROW
- Data on overdoses and drug use drive targeted response.
- Proactively going door to door in high-risk neighborhoods helps prevent overdoses.
- Including peer supporters amplifies impact.
- Resource information and sharing should include pushing for one specific action.
Each team of individuals that knocks on doors usually consists of no more than three or four people, including one law enforcement representative. The officer approaches the targeted home first, both to ensure the safety of volunteers and to break down barriers between law enforcement and the community. In addition to an officer, the team often includes a representative from Cornerstone, a representative from a local community center, and a peer support specialist. Three peer supporters are full-time GROW employees, two of whose salaries are paid for by a grant from the Ohio attorney general’s office and one of whose is paid for by Cornerstone.64
On a blitz, the volunteer team speaks to anyone who will listen. This might include the person who has overdosed, friends or family members, or a concerned neighbor. Volunteers share a bag of resources with residents and leave a door knocker with pertinent information at doors that are unanswered. Resource bags contain information on various recovery services—including medication-assisted treatment providers, Narcotics Anonymous, and faith-based treatment providers—business cards for GROW staff and volunteers, and a referral form for the Cornerstone Front Door initiative. Volunteers talk about the Cornerstone Front Door initiative, promising that anyone who seeks help from Cornerstone will be seen the same day.
In 2017, GROW visited 311 homes, made contact with 190 individuals, and referred 21 people to treatment. In 2018, GROW increased its operations; in the first half of the year, GROW visited 423 homes, held 205 conversations, and left 221 door knockers at unanswered doors.65
GROW has also had an impact on the sheriff’s deputies and officers who participate. Working directly with individuals affected by addiction has helped change officers’ perceptions and break down the stigma associated with addiction. And importantly, GROW provides deputies with a pathway to support individuals with substance use disorders. Law enforcement previously had few options for responding to risky substance use behaviors that were short of taking the individual to jail. Now, officers can follow up with GROW staff after an interaction and refer an individual for outreach. This happens more and more frequently.
Moving forward, the Drug Enforcement Agency (DEA) may provide funds to expand GROW outside of Montgomery Country through its DEA 360 Strategy, an initiative that includes community outreach through partnerships with state and local entities.66 Consideration is being given to the feasibility of including training on how to support those in active addiction for police academy students.
The Montgomery County Drug-Free Coalition hosts town hall meetings at community churches, which often funnels volunteers to GROW. At the town hall meetings, the sheriff or a deputy shares context on the epidemic, provides an overview of services their department provides, describes treatment options in the county, and solicits volunteers. This outreach has resulted in hundreds of individuals volunteering to participate in GROW blitzes and going door to door to share treatment information.
Mobile Crisis Response Team
Another key element of the city’s effort to bring services directly into the community is the DPD’s Mobile Crisis Response Team. Like GROW, the Mobile Crisis Response Team conducts outreach to individuals with substance use disorders and supports them in accessing treatment. The initiative also grew out of the volunteer effort, described above, to visit residents impacted by overdoses, spearheaded by a police officer and partners within the community.
Today, the Mobile Crisis Response Team consists of three dedicated police officers, two of whom are focused on responding to mental health crises and one of whom is versed on issues related to addiction. The role of addiction officer, which requires training in mental health first aid and crisis intervention, became a full-time position with the department in December 2016. The position was intially part-time for approximately six months. Officers are joined by an emergency medical technician from the Dayton Fire Department, who has been a full-time member of the team since August 2017, as well as participants from Peers for Change.
No day looks the same, as the team’s response is tailored to individual needs and interactions. They typically start their day by reviewing the daily automated list, mentioned previously, of individuals who have overdosed. The team notes additional individuals it intends to follow up with based on past days’ work. Next, the team builds a route to visit the selected individuals.
Though the team members begin with a plan, they are prepared to deviate from it if a more pressing need arises. They respond immediately if an individual with substance use disorder or their family member contacts the team asking for help entering treatment. Team members also respond immediately to overdoses in process, either at the location of the incident or at the hospital.
Compassion and knowledge of substance use disorder guide each conversation. Team members understand that addiction is a chronic illness. They understand the likelihood of relapse and that it may take many treatment attempts before someone remains in recovery. They also understand the stigma around addiction and that those suffering from the disease and their family members often lack people in whom they can confide. This knowledge guides the team’s work.
Key lessons learned: Mobile Crisis Response Team
- Similar positions should be full-time to build systemic knowledge.
- It takes time to build comprehensive understanding of treatment options.
- It is very difficult for people to commit to entering treatment, but reducing logistical barriers helps.
- Officers must commit to building long-term relationships with the people they work with.
- Officers should let those they interact with guide the conversation.
- Navigating health insurance is a central component in helping people access treatment.
When the team arrives at a home, they knock on the door and ask for the individual they have targeted for a visit. They preface their requests by explaining that this person is not in trouble. Rather, they explain that they are there because they believe the person is in need and they want to help. If the person is not present, the team speaks to whomever answers the door—that is, if that person is willing. The team shares their business cards and treatment resources, explains that they are here to help anyone who needs it, and emphasizes that this work is their job. Team members are also prepared to furnish family or friends with Narcan and train them on how to use it if requested. If no one is home, they leave a resource bag and their contact information at the door.
If the person who overdosed is present, the conversation could go in many different directions. On one recent visit, the person who had overdosed said that he had not really overdosed—that he was just physically exhausted. The officer did not argue, even though he was aware that the man had been revived with multiple doses of Narcan. Instead, the officer gently explained the team’s job, shared their contact information, and stated that the team was here to help if he ever needed it. Though the man never acknowledged his overdose or addiction, he clarified that he could contact the team if he needed help.
At a second home, a peer supporter spoke with an individual with substance use disorder while the officer spoke with this individual’s stepfather. The individual indicated that she did not want to speak to the peer supporter. At that point, the peer supporter accepted her answer and walked away. It was clear in each instance that it is important to let the individual guide the conversation.
The officer rejoined the individual in need, and she agreed to answer some follow-up questions, as she knew the officer from prior outreach efforts. The officer had previously helped her to enter treatment, but the individual shared that she did not want to go into treatment again. When the officer asked why, she shared that she would have nowhere to go once she got out of treatment. He pressed further, saying that his team could assist her in locating sober living once she graduated from a treatment program. The woman again said that would not work and that there were too many drugs in Dayton for her to be successful. The officer pressed once more and said they could help her find treatment outside of the city. She declined, but he reminded her to contact the team if she changed her mind. In this case, the officer leveraged the existing relationship to gather information and demonstrate the team’s ability to minimize barriers to entering treatment and remaining in recovery.
The Mobile Crisis Response Team estimates that someone expresses to them a desire to enter treatment at least once a day. Once someone decides he or she wants help accessing treatment, the team enters the conversation recognizing that it still may take time. For example, the team may first need to assist the individual in gaining health insurance. They might next spend time with that person discussing treatment options. After several additional conversations, the person might be fully ready to enter treatment.
The team believes that one of its greatest value-adds is its ability to seamlessly assist individuals in navigating treatment. Accessing treatment is often complicated. It requires finding an open bed and understanding one’s health insurance, as well as knowing various details about treatment providers. This includes any details that would exclude someone from treatment, what health insurance is accepted, and which services are offered.
Entering treatment would be difficult for most people, but the difficulty is exacerbated for people who may be experiencing withdrawal, cravings, or anxiety. The challenges are even greater for the nearly 40 percent of people with a substance use disorder who also suffer from mental health disorders.67
When the team first began this work, navigating treatment options and helping people enter treatment was a huge hurdle. One of their biggest accomplishments is developing relationships at centers in the region and across the state. The time the team has put into helping others find treatment has resulted in advanced knowledge of available treatment providers and strong relationships with individuals at each center. The team’s contacts at various treatment locations assist them in hastening the entry process, meaning they are now typically able to get individuals into treatment the same day an individual requests help. This process is streamlined for the team but not necessarily for the average community member. There is much work to be done to make the treatment system more widely accessible.
The Mobile Crisis Response Team does whatever it takes to assist individuals in entering treatment. Securing transportation is a challenge for many, so they often drive people to local treatment centers themselves in a police cruiser. They work to secure a ride for the individual if they are working with many people at once or for distant destinations. This may mean riding with a loved one or securing a vehicle for hire.
A commitment to developing long-term relationships is central to this work. Team members have known many of the individuals they support for months, visiting some nearly every day. Some clients enter treatment after months of conversation and outreach.
The team also understands that people usually make multiple attempts at treatment and that those in recovery also need support post-treatment. The team therefore commits to the long term even for those they meet briefly. They initiate conversations about post-treatment support before someone begins treatment, sharing that the team can help make connections to sober living or in regaining custody of children. They also follow up with individuals who are in treatment. For instance, team members visited one man who recently entered outpatient treatment to find out if he was still attending and to hear about his experience. He had already gone to treatment for the day, so the team left a message to let him know they had been there and were thinking of him.
This sort of commitment also means the team is immersed in the city’s recovery and advocacy communities and versed in the county’s efforts to combat the opioid epidemic. They regularly attend other organizations’ events and participate in GROW blitzes throughout the county. They share information across agencies and form relationships with peer supporters. This is an important component in helping to foster a community that will support individuals into and beyond treatment.
Over a 17-month period from January 2017 through May 2018, the team responded to 266 overdose calls, followed up on 851 overdoses, made contact with 370 victims, connected with 406 family members or friends of victims, and referred 152 individuals to treatment.68
The team has learned several important lessons through these contacts. First, they have learned to observe how peer supporters interact with individuals in active addiction. Second, they have learned not to persistently challenge people who are not ready to enter treatment. Only when someone is ready to enter treatment is it appropriate to challenge excuses that arise and may be grounded in fear. Third, they have learned to let the individual guide the conversation. Though police officers are often inclined to ask lots of questions, they have learned that it is often more effective to hold back and listen. Team members have found that individuals they meet are ready to talk and often share more if they are not pressed with questions.
The team has plenty of work to do in the city. They believe that at least one more full-time officer would have ample responsibilities and advance the work if budget permitted. Any person beginning similar work must be prepared to lead with compassion and commitment to the work. The team has found that individuals in active addiction quickly recognize when someone is disingenuous or not fully committed to the work.
Finally, the team actively seeks to combat the stigma around addiction. This comes through in nearly every conversation team members have, whether with community members or peers in law enforcement. The team speaks from their own experience, describing addiction as a disease and the immense challenges around entering treatment. They also share in the belief that their work assists the fire and police departments by reducing overdose calls and that the conversation around addiction is changing in the community and among their peers.
Cornerstone Front Door Initiative
The Cornerstone Front Door Initiative is a public-private partnership between the Cornerstone Project, East End, and various law enforcement agencies that was designed to provide a warm handoff between law enforcement and treatment providers. Individuals who come to the Front Door with a GROW referral form or are brought in by law enforcement are seen by a clinician within 24 hours to 48 hours.
The program was launched in the spring of 2016 as part of the Byrne Criminal Justice Innovation Grant. It is housed in East Dayton, the neighborhood that is most heavily impacted by the opioid epidemic. Although there was previously no treatment center in East Dayton—despite the need for one—it was still challenging to launch the Cornerstone Front Door Initiative. Residents often resist having treatment centers in their communities due to the stigmas surrounding addiction and misperceptions that crime will increase as a result. The partners worked closely with the neighborhood association to bring the project to fruition, addressing concerns by adding lighting in the area and installing surveillance cameras, which the Dayton Police and Fire departments monitor.
Key lessons learned: Cornerstone Front Door
- A dedicated law enforcement line is an effective tool for a warm handoff.
- High-risk communities must have physical access to treatment.
- Helping someone enter treatment is often a collaborative, multi-intervention effort.
Because Cornerstone Front Door provides a dedicated law enforcement phone line, when an officer or deputy encounters an individual willing to seek treatment, they can bring the individual directly to the center. This eliminates the obstacle of securing transportation to treatment, which is a challenge that many individuals in need face, and provides an alternative to incarceration. If individuals arrive after hours, Cornerstone attempts to connect them to a sober-living facility until the center reopens. If there are no beds available at a sober-living facility, Cornerstone Front Door works with the individual and law enforcement to arrange for the individual to be picked up and brought to the center as soon it reopens. Early on, Cornerstone Front Door struggled to navigate situations where individuals did not have appropriate health insurance or where individuals agreed to enter treatment only because it meant that their legal charges would be dropped. Cornerstone Front Door found that these individuals often left treatment soon after arriving. Additionally, some police officers attempted to arrest individuals who were in treatment. As a result, Cornerstone developed individual policies and procedures for each partner community, tailored to meet the needs and context of that community. They also built a protocol for working through arrest warrants for individuals in treatment. Now, law enforcement works through a Cornerstone point person rather than entering the treatment facility.
Case study in community interventions: Colleen’s story
One story illustrates the collaborative efforts of the community. The day Cornerstone Front Door opened coincided with a law enforcement blitz targeting drug dealers. Colleen, whose name has been changed to protect her anonymity, watched the blitz in action and tried to dispose of needles she was carrying while in the vicinity of the Cornerstone Front Door building. Police had observed her, however, and she was arrested.
Colleen was in great need of help. She had experienced multiple overdoses and had been physically and sexually exploited. Colleen wanted to seek treatment at Cornerstone Front Door, yet she now associated the location with law enforcement and her arrest. And while she would not enter treatment, she nonetheless began forging a relationship with various members of the recovery community, including Cornerstone’s community outreach coordinator. Starting in 2016, Colleen visited Cornerstone Front Door about once a week to receive a meal and spend time with the coordinator. Peer supporters reached out to Colleen, and the Mobile Crisis Response Team visited her nearly every day, offering food and information on treatment.
In July 2018, Colleen sought out the Mobile Crisis Response Team and indicated she was ready to enter treatment. Everyone involved was thrilled that she took that first step, although it is understood that it may take multiple attempts before Colleen remains in recovery. All those involved know that patience is key in such work, and although they may want an individual to enter treatment and recovery, they must wait until that individual is ready. Two years ago, Colleen was not ready—but today she is.
Not only is patience integral to successful outreach work, but Colleen’s story also demonstrates the importance of developing long-term relationships with individuals suffering from addiction. Colleen’s experience serves as further evidence of the value of an all-hands-on-deck approach. If Cornerstone Front Door, Peers For Change, or the Mobile Crisis Response Team had viewed Colleen as someone else’s client or responsibility, she may not have decided to enter treatment in July. Instead, their collaborative effort provided Colleen with a community of support.
The Montgomery County Jail
Before 2016, providing services to incarcerated individuals was a significant gap in the continuum of care for two primary reasons. First, Medicaid benefits are suspended when an individual enters jail. Second, people who had been receiving treatment for substance misuse were not able to continue to access those resources once they entered jail. This led to high rates of relapse and overdose upon exiting the Montgomery County jail.
Key lessons learned: Montgomery County Jail
- Treatment services must not be cut off when someone is incarcerated.
- Receiving medication-assisted treatment and connections to treatment providers prior to re-entry helps reduce risk of overdose and death.
As a result, the county’s Alcohol, Drug Addiction, and Mental Health Services (ADAMHS) funded behavioral health screening and assessment services within the jail beginning in 2016. ADAMHS recently contracted out those services to a central provider. More recently, they have added Medication-Assisted Treatment (MAT), an approach that pairs behavioral therapy with prescription medications that alleviate the symptoms of opiate withdrawal to help patients safely overcome addiction. Other treatment providers provide additional services to incarcerated individuals when the contracted agency is unable to meet the population’s needs. Behavioral health providers who already have a relationship with an incarcerated patient may continue service while they are in jail. The jail also has two peer supporters who support incarcerated individuals and connect them to services.
To better integrate services, the county jail employs a full-time coordinator to identify needs and gaps in services; connect incarcerated people to their parole officers and maintain communication; identify individuals in need of assessment; and determine whether individuals had a treatment provider before incarceration.
Currently, treatment providers meet with their clients in the jail, and ADAMHS funds the services provided. Finally, a state grant funds the coordinator and treatment providers to assist clients in accessing housing and other services as they prepare for re-entry.
Awareness and treatment through Montgomery County ADAMHS
Education and awareness outreach
ADAMHS uses multimedia outreach to educate the community about issues related to substance use disorders, from helping residents better understand and support their loved ones to raising awareness about dangerous events such as a bad batch of drugs on the street.
One way ADAMHS seeks to arm the community to act is through its free smart phone app, called GetHelpNow Montgomery County. This app assists in locating addiction and mental health resources, housing, and other services. ADAMHS, like other local organizations, recognized that many people did not know where to turn once they were prepared to enter treatment. The app is one attempt to remove barriers to accessing treatment, allowing family members and friends to understand the options available even before their loved one is prepared for treatment. Since launching, the app has received an average of between 10 uses and 20 uses per day.
Residential treatment and detoxification services
Residential treatment beds in the county have increased over the past several years. On average, new patients now enter residential treatment on the same day that they seek treatment.
In 2017, ADAMHS identified a gap in treatment for individuals with dual diagnosis, who simultaneously experience mental health and substance use disorders.69 For these individuals, wait time averaged between three weeks and six weeks for treatment. To address this problem, ADAMHS worked with one of its contracted providers to relocate dual diagnosis beds from a smaller location to their main campus. This allowed for the expansion of their service, reducing the wait time to two days. The transition only took about four months.
Key lessons learned: ADAMHS
- Provide opportunities for loved ones to increase their knowledge around treatment options even before their loved one is ready for treatment.
- Dual diagnosis beds must meet community needs.
- Communities must have detoxification beds.
ADAMHS funds assistance for individuals unable to pay for service. Typically, it is easiest to find treatment coverage for people with Medicaid, followed by those with private insurance. Medicare tends to be the most difficult. ADAMHS steps in as a last resort payer to provide for those without coverage. These funds are provided through Montgomery County’s human services levy.
The county also has a gap in detoxification beds for individuals going through withdrawal. As a result, ADAMHS has partnered with the county commissioners and local hospitals to develop a crisis stabilization unit, set to open by January 2019 with operational plans for the first five years. The unit will provide detoxification services as well as observation for up to 23 hours for individuals in crisis but without a clear diagnosis. This unit will also serve as a hub to connect individuals to longer-term treatment options.
Harm reduction initiatives
Harm reduction strategies aim to reduce the dangers associated with drug use by promoting safer substance use behaviors. Harm reduction focuses on improving the well-being of individuals who are not yet ready to enter treatment by preventing overdose fatalities and limiting the transmission of disease.
Narcan use and distribution
The city of Dayton’s first responders are on the front lines of the opioid epidemic. In 2017, Dayton Police and Fire departments responded to more than 3,400 calls for service related to overdoses. In the first six months of 2018, they responded to 922 overdoses.
Many of these calls require first responders to administer the lifesaving drug naloxone, sold under the brandname Narcan. The Dayton Fire department has administered Narcan since 1979, and the DPD has administered Narcan since 2014. It was one of the first police departments in Ohio to do so following a change to state law that permitted police to carry the drug. The DPD also trains surrounding jurisdictions in the use of Narcan.
Key lessons learned: Narcan
- Narcan saves lives.
- Drug users often use together, so disbursing Narcan to those who want it helps friends save one another’s lives.
Some community members, politicians, and law enforcement in Ohio have suggested that unlimited provision of Narcan will encourage opioid users to take risks, knowing they will be revived if they overdose. There is absolutely no evidence supporting this argument, however. Instead, the evidence shows that Narcan saves lives. The nature of addiction means that people continue to use until they are prepared to receive treatment, so not providing Narcan would not be a use deterrent. The CDC recommends naloxone use as a best practice.70 Furthermore, a 2017 National Bureau of Economic Research study identified a 9 percent to 11 percent decrease in opioid-related deaths in areas with increased access to naloxone.71
ADAMHS’ executive director explained that the misconceptions around Narcan are often rooted in the stigma around addiction. Narcan is first aid for someone in crisis and must ultimately be as accessible as a bandage for an injury.
Since 2015, Dayton Police and Fire departments have administered more than 24,000 milligrams of Narcan in more than 7,300 overdoses. From 2014 to 2016, approximately 95 percent of individuals who received Narcan from the DPD were revived.72
While it is difficult to determine Narcan’s precise level of impact due to additional factors such as drug potency, evidence suggests that Narcan contributed to the declining numbers of overdoses in late 2017 and the first half of 2018. Figure 10 compares the amount of Narcan administered, number of overdoses, and number of overdose deaths for the first six months of the years 2016 and 2018. The number of overdoses in the first six months of 2018 were about the same as in 2016, but overdose deaths were almost 40 percent higher in 2016. Notably, Narcan delivered is higher in 2018, suggesting higher dosages delivered saves lives.
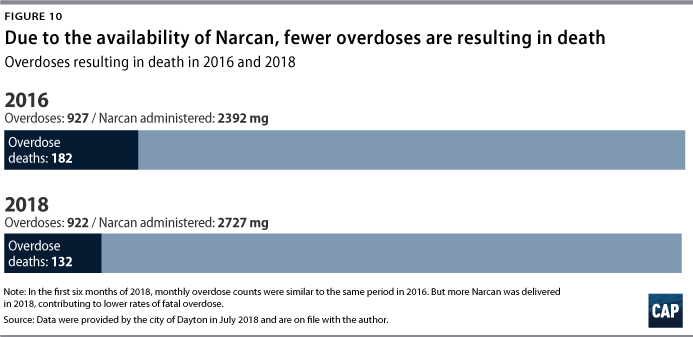
A dose of Narcan costs approximately $40 per two milligram dose. Since 2015, the city of Dayton has delivered more than $500,000 in Narcan in response to overdoses. ADAMHS and Public Health fund the Narcan. (see breakdown of overdose responses and spending below)
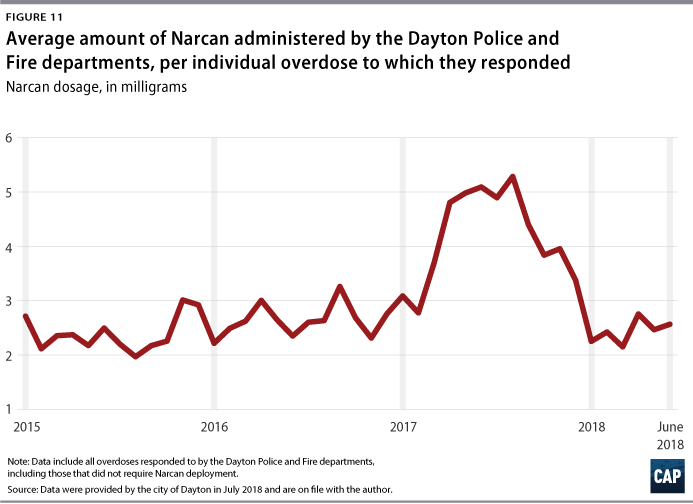
As fentanyl became more widespread, the amount of Narcan required to reverse a person’s overdose increased, and overdose deaths spiked. Fentanyl was involved in 41 percent of deaths in 2015, but by 2017, it was involved in 64 percent of deaths. At the same time, first responders have witnessed an increase in the average dosage of Narcan required to reverse an individual’s overdose. 73 Figure 16 shows the increase in Narcan required per person. Though deaths declined in the latter half of 2017, Narcan dosage required remained high.74

GROW, the Mobile Crisis Response Team, Conversations for Change, and CarePoint all furnish Narcan to the public. In 2017, Public Health and Project DAWN partnered to train employers on how to use Narcan and share Narcan with businesses that wished to keep Narcan on site. Public Health also initiated an Overdose Outreach Program which supports individuals who have overdosed and their families. In 2017, more than 3,700 Narcan kits were distributed to the public.75
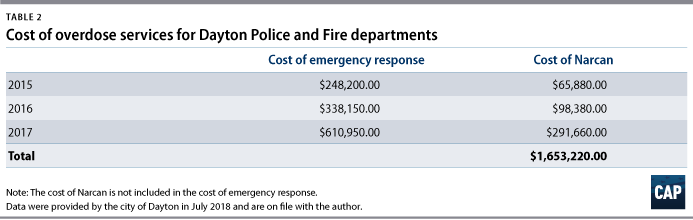

CarePoint syringe services
In late 2014, Public Health and the city of Dayton initiated plans to open a syringe exchange program in partnership with the Life Enrichment Center, the AIDS Resource Center Ohio, ADAMHS, Montgomery County, and the DPD. At the time, used needles and syringes often littered public spaces; police officers had been stuck with used injection equipment during pat downs; and concerns about blood-borne infections were on the rise.
The above group convened early in the epidemic, recognizing that a syringe exchange program would offer a safe way to dispose of used syringes and reduce harm caused to individuals using intravenous drugs. Because Public Health did not have strong data demonstrating the incidence of hepatitis C or HIV, there was initially some skepticism around the need for such a program. Ultimately, the partners agreed to pilot the program for six months, before fully expanding it if successful.
At the time, a syringe exchange program could only be opened if the region was experiencing a state of emergency. The city of Dayton therefore declared a state of emergency related to injection drug use on February 19, 2015. This declaration permitted the creation of CarePoint Syringe Services Program, which opened in April 2015.
Key lessons learned: CarePoint
- Start small when first opening a syringe exchange service, and only provide other services that are very routine for the provider.
- Retaining staff is an essential element in connecting clients to services beyond syringe exchange.
- Public relations and garnering community support is essential to maintain a syringe exchange program.
- Partner with law enforcement to determine policies for drug paraphernalia.
Stigma abounds around needle exchanges. Many people incorrectly believe that such programs encourage illicit drug use. Others believe drug users to be violent or dangerous and therefore do not wish to have exchanges in their neighborhoods. Yet, studies show that syringe service programs do not encourage drug use or increase illegal activity.76 In fact, public health experts—from the American Medical Association to the CDC—recommend syringe exchange programs as a tool to combat the spread of HIV.77 Not only can syringe exchanges save lives, but they also have the potential to save taxpayer dollars: It costs less to implement a syringe exchange program than it does to treat long-term infections such as HIV.78 One study found that a $1 investment in syringe exchange programs saved at least $6 in averted costs of HIV treatment.79
Finding a location for Montgomery County’s program was challenging, in part due to this stigma. Residential neighborhoods often did not want to host such sites. Additionally, legal requirements at the time prevented the operation of syringe access programs near schools or daycares. Public Health and the city initially identified promising locations only to find that they would not meet the legal requirements.
Finally, Dayton’s Life Enrichment Center (LEC) was selected as the site for the syringe exchange program. Not only did the location meet the legal requirements, but LEC is conveniently situated between the eastern and northern neighborhoods, which meant it would be accessible to two of the areas with highest concentrations of substance misuse. Importantly, LEC leadership was on board with the idea. LEC’s director was interested in hosting the program as a way to connect clients to the other services provided at the center. In addition, Public Health had an established relationship with the director and sponsored existing programs at the LEC.
Securing and maintaining community support was integral to launching the program and ensuring its continued success. One way that organizers sought to cultivate community support was by seeking buy-in from business owners in the LEC neighborhood. They held a luncheon prior to the program’s opening to educate business owners on the goals of harm reduction. They described the premise for the program: It is modeled off a syringe exchange site in Green Bay, Wisconsin, one of the largest programs of its kind in the country.80 The director of the LEC also described benefits to the business leaders, explaining that employees could very well be the same people who need these services.
The program’s goal is to reduce harm for those using intravenous drugs by providing a one-for-one exchange of clean syringes for used ones. It is important to note, however, that one-to-one exchanges differ from an open access model, which provides clients with an unlimited number of syringes without requiring the disposal of a used one. The one-for-one exchange model was selected by a group of stakeholders and citizens that met in the early stages of developing the program. In part, the strategy helps preserve community buy-in, as the program collects as many syringes as it is provides. There has been a resulting decline in reports of syringes on the streets or in parks. While unlimited syringe access is described as a best practice for preventing individuals from sharing injection equipment, the one-for-one exchange model has worked for Dayton.
CarePoint filled a significant gap in the community. In 2017, more than three-fourths of CarePoint’s new clients reported they did not otherwise have access to sterile syringes, so this service was greatly needed.81 The Public Health staff first complemented the syringe exchange program with services they already did well rather than attempting to try many new things all at once. After starting small, they gradually provided additional programs, such as Medicaid enrollment-assistance and Narcan disbursement.
After its initial successes, the program expanded to two additional locations, Narcan services were added in 2016, and a mobile unit was opened in April 2018. The program distributes contraception, cotton balls, cookers, and tourniquets to better prevent the transmission of infections. Clients are offered referrals to recovery services; medical and dental care; mental health care; on-site medical testing for pregnancy, syphilis, hepatitis C, and HIV; on-site Medicaid enrollment assistance; and a number of social services provided by the LEC.
Public Health provides funds and staff for CarePoint. Employees chosen to lead the program had decades of experience working with individuals using intravenous drugs through prior Public Health programs around HIV prevention and education. This meant the staff already had rapport and trust with several clients within the community. The staff has remained constant since the program’s inception. Retention has been a key element in forming trusting relationships with clients. Once staff have seen someone a few times, it makes it easier to truly begin discussing other services and treatment options.
Ensuring law enforcement buy-in was an important element in CarePoint’s success. A representative of the police department was instrumental in the initial planning for the program. The officer helped to determine that the Wisconsin model could likely work in Dayton. The officer also served as an advocate within the police department, helping to educate other officers on the rationale for the program and on how to interact with CarePoint’s clients. When the center was first opened, officers arrested some clients for possession of hypodermic needles, paraphernalia related to drug use. To ensure that clients could safely seek CarePoint’s services without fear of arrest, CarePoint now provides each new client with an ID card that uses an ID number in lieu of the client’s name to protect anonymity. As long as a client is carrying a CarePoint ID card, they cannot be arrested for possessing injection equipment.
The program is strict about on-site drug use, and it clearly and directly tells clients that they are not allowed to use on site. They also do not permit people to use the bathroom when visiting for syringe services, as public bathrooms are a common site for drug use. Finally, employees patrol the parking lot to ensure no one is using illicit drugs on the property.
New clients complete a comprehensive and confidential questionnaire. This provides important insight into the clientele, including demographic information, housing and health insurance status, mental health and medical history, and drug use history.
CarePoint’s clients are primarily white, split nearly evenly between men and women, and have an average age of 37 years old. Of new clients in 2017, 64 percent were unemployed and 13 percent received disability benefits. Nearly all clients indicated that they primarily use opioids, and 37 percent of new clients reported being diagnosed with a mental health disorder in their lifetime. Of those diagnosed with a mental health disorder, more than 80 percent reported being prescribed medication for their disorder, but only one-fifth reported taking the medication.82 The survey provides extensive knowledge of clients’ needs that can aid in assessing gaps in service and in developing further services.
The program has seen significant use and success throughout its existence. The following are prime examples of the program’s impact:
- 125,383 syringes were exchanged in 2017. In the first five months of 2018, 81,361 syringes had been exchanged. If this trend continues, more than 195,000 syringes will be exchanged by the end of 2018.
- CarePoint had 4,945 encounters with clients in 2017. From January to May 2018, there were 2,363 encounters. Encounters will outpace those in 2017 if this trend continues.
- CarePoint has made 240 referrals to drug treatment since beginning its operations.
- 6 percent of new clients reported hearing about CarePoint through outreach in 2016. By 2018, this number dropped to 15.4 percent, and 79.1 percent report they learned about the program through a friend.
- CarePoint has distributed more than 2,052 Narcan kits. More than 70 percent of those receiving the kits report that the kit is for self use. Most of those requesting a refill report that their kit was used rather than expired or lost.
Dayton’s original syringe exchange sites have been successful, but it has been a challenge to expand into the rest of Montgomery County. The county’s mixture of urban, rural, and suburban towns creates a complex landscape. The mobile unit is ready to go, but the more rural communities have been less open to allowing syringe exchange services. In part, this is because it is often more difficult to recognize the extent of the problem in towns with small, diffuse populations. Public Health has not yet been able to garner broad support for syringe services throughout the county.
Conclusion
Dayton and Montgomery County have made important strides in tackling the opioid epidemic in the region. The efforts outlined in this report have saved lives and helped people return to the lives they once led.
Knowledge around addiction as an illness undergirds the community’s actions in and around Dayton. Communities cannot hope to mount an effective response without this foundational knowledge. Similarly, knowledge leads to increased compassion and the ability to combat stigma. These mindsets must be at the core of any successful response to address the opioid crisis.
In Dayton, data drive nearly every intervention. These data are intentionally captured, rapidly released, and thoughtfully deployed to take action. That said, people in Dayton did not wait for data to come in before they began acting. In some cases, grassroots organizing came first, and data collection came later. Rather than waiting for local data to drive a response, communities should look to cities such as Dayton for effective responses.
A crisis response requires individuals, organizations, and agencies to step out of their traditional roles and comfort zones. For Montgomery County, this meant learning how to organize many diverse groups and agencies around a collective impact model. It also meant taking services directly to the people and trying new techniques and testing ideas without the fear of failure.
Opportunities abound to continue to improve the response to the opioid epidemic. First, there must be additional opportunities for harm reduction for those who are not prepared to enter treatment. Second, the continuum of care must be improved. For example, there could be even more outreach and support provided to help individuals enter treatment, access medication-assisted treatment, and remain in recovery. Finally, the stigma around addiction and mental health disorders must be further reduced.
The coordinated response to the opioid epidemic means that the community is better poised to respond to addiction, regardless of the drug. It has also opened an important discussion around mental illness. The lessons learned will therefore continue to evolve and impact Daytonians for years to come.
About the author
Erin Welch wrote this report in memory of her brother, Sean Francis Welch. Welch is passionate about ensuring expansive access to mental health and substance use services and fighting to eliminate the stigma around mental health and addiction. She received a Masters of Public Policy and Management from Carnegie Mellon University in December 2018 and holds a Bachelor of Arts from Cornell University. Before returning to school, Welch was the director of licensure and regional operations at Teach For America in Arkansas. There, she worked with admitted applicants as they transitioned into their new roles as teachers in the Arkansas Delta and oversaw their placement with partner communities. She was the liaison between Teach For America and the Arkansas Department of Education, ensuring all teachers within the region were fully licensed. She also administered the region’s AmeriCorps grant. Welch was a founding board member of GLSEN Arkansas, an organization that seeks to create safe, welcoming schools for LGBTQ students. Prior to her work in Arkansas, she completed two years of full-time service as an AmeriCorps member with City Year Columbus.
Acknowledgements
Many individuals in Montgomery County contributed to the writing of this report. This report would not be possible without Dayton Mayor Nan Whaley, her love for her community, and her drive to ensure Dayton’s story is told and shared. The author would like to particularly thank Officer Jason Olson and Emergency Medical Technician Amy Dunkin, who provided a wealth of information and allowed her to join them in their work. In addition, Major Brian Johns was an ongoing resource and support. Ariel Walker and Torey Hollingsworth provided feedback and guidance throughout the writing process, and Laura Pippenger edited the document.
The following interviews, meetings, and events deeply informed the report. The author would like to thank all those who contributed.
- Major Brian Johns, Dayton Police Department, June 7, 2018
- Jeff Cooper, commissioner of Public Health, and Barbara Marsh, assistant commissioner of Public Health, Public Health of Dayton and Montgomery County, June 13, 2018
- Officer Jason Olson, Dayton Police Department, and Emergency Medical Technical Amy Dunkin, Dayton Fire Department, June 14, 2018
- COAT Prescription Opioid Branch meeting, June 22, 2018
- Families of Addicts Help Summit: The Secret Affecting Your Bottom Line, June 27, 2018
- GROW blitz, Harrison Township, June 28, 2018
- Officer Jason Olson, Dayton Police Department, and Darcy Shepherd, Peers for Change, July 2, 2018
- Wendie Jackson, Cornerstone Project community outreach manager and director of GROW, July 5, 2018
- Helen Jones-Kelley, executive director, Montgomery County ADAMHS, July 10, 2018
- Public Health and ADAMHS release of Crescendo Report on Behavioral Health, July 10, 2018
- Emily Surico, East End Community Services, July 11, 2018
- Janine Howard, director, Health Services; Andrea Young, AIDS program supervisor; Joyce Close, bureau supervisor, Communicable Disease; Public Health of Dayton and Montgomery County, July 17, 2018
- Sheriff Phil Plummer, Montgomery County Sheriff’s Office, July 17, 2018
- Families of Addicts Dayton meeting, July 18, 2018
This report was created with support from the John D. and Catherine T. MacArthur Foundation as part of the Safety and Justice Challenge, which seeks to reduce over-incarceration by changing the way America thinks about and uses jails.