The American Health Care Act (AHCA) as passed by the House of Representatives would slash subsidies and repeal other federal policies that help make health coverage affordable nationwide. Two particularly notable consequences of the House-passed bill would be widespread premium hikes in 2018 and severe premium increases for older Americans in 2026.
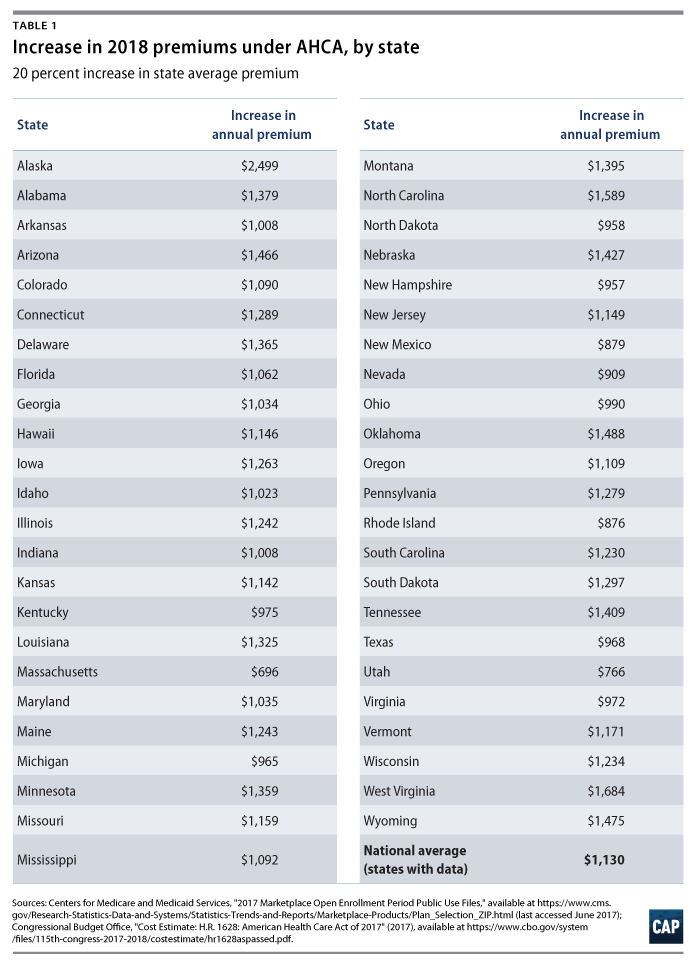
The effect of the AHCA on premiums would be almost immediate. The Congressional Budget Office (CBO) estimates that the AHCA would increase individual market premiums by 20 percent in 2018, largely due to elimination of the individual mandate. The Center for American Progress estimates that this 20 percent rate hike would increase the average annual premium in the marketplace by $1,130 in 2018. These 2018 premium increases would vary by state, as shown in Table 1, from a $766 increase in the average in Utah to $2,449 increase in the average in Alaska.*
In addition to overall rate hikes in the near term, older Americans would face massive premium increases over the next decade due to the AHCA. This is because the AHCA would weaken the Affordable Care Act’s (ACA) rule that limits how much insurers can vary premiums based on age. The AHCA would allow insurers to charge older enrollees five times more than younger enrollees starting in 2018, as opposed to three times as much under current law.
AARP, among other consumer groups, has criticized the AHCA’s wider age band as an age tax that would make it harder for near-elderly people to afford health care. The Senate’s version of the bill is currently also expected to allow higher premiums for near-elderly people.
The policy would hurt low-income individuals the most. Although the AHCA provides premium tax credits that would increase along with age, the subsidies would be insufficient to make up the difference in premiums for older Americans. After taking into account available tax credits, the CBO projected that in 2026, the annual premium for a 64-year-old individual with a low-middle income of $26,500 would be $1,700 under the current law but would soar to $16,100 under the AHCA.
CAP estimated the net premium increases that near-elderly enrollees would face under the AHCA’s age tax relative to under the ACA in each state. We used government data to calculate how much higher or lower each state’s average 2017 benchmark silver premiums would be compared with the overall average.** We then used those factors to adjust the CBO 2026 projected premium for the states that would continue to maintain protections for people with pre-existing conditions and require plans to cover the ACA essential health benefits.
Under the ACA, premium tax credits would automatically adjust such that a 64-year-old with an income of $26,500 would pay only $1,700 for silver benchmark coverage in any state in 2026. By contrast, the AHCA tax credits would be fixed, and their generosity would not vary to account for local premium costs.
Estimates for all states with available data are available below in Table 2. For example, the average 64-year-old West Virginian making an income of $26,500 in 2026 would pay a net premium of $22,400 per year under the AHCA, compared with just $1,700 per year under the ACA—a $20,700 increase in annual costs. The age tax would be much higher in states where health care costs are high. The ACA subsidies would ensure that a similar Alaskan would pay only $1,700 for coverage, but under the AHCA, that person would owe $49,070 toward coverage. Thus, the AHCA’s age tax in Alaska would be more than $47,000 per year.

As these estimates demonstrate, the AHCA would drive sharp rate hikes for all individual market enrollees starting next year and would make health care prohibitively expensive for older enrollees. Simply put, the AHCA would make health coverage harder, if not impossible, to afford for millions of Americans.
Emily Gee is the health economist for the Health Policy team at the Center for American Progress. Thomas Huelskoetter is the policy analyst for the Health Policy team.
* Our 2018 rate increase analysis is limited to the states that reported an average 2017 premium to the Centers for Medicare and Medicaid Services.
** This analysis is limited to the states included in the report on 2017 benchmark rates by the U.S. Department of Health and Human Services.